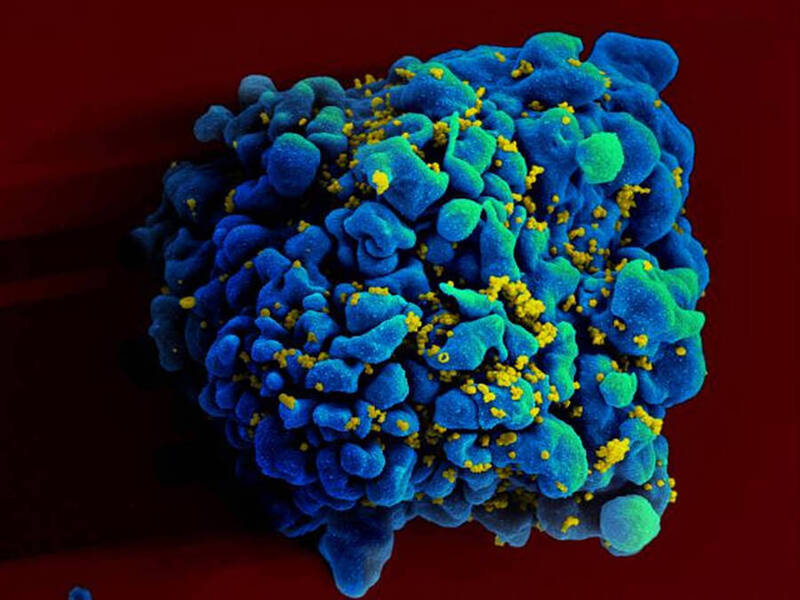
In Oslo, Norway, a man living with HIV for over two decades achieved sustained remission after receiving a stem cell transplant from his brother, who carries a rare CCR5-delta 32 genetic mutation that confers natural resistance to HIV infection, marking only the fifth documented case globally of HIV remission following such a procedure.
The Genetic Shield: How CCR5-Delta 32 Blocks HIV Entry
The CCR5 receptor on CD4+ T cells serves as a primary co-receptor for HIV-1 to enter and infect immune cells. Individuals homozygous for the CCR5-delta 32 mutation lack functional CCR5 receptors, preventing most strains of HIV from establishing infection. This man’s brother was heterozygous for the mutation, meaning he carried one copy of the delta 32 allele, which still conferred sufficient resistance to produce his stem cells a viable donor source. The transplant replaced the patient’s HIV-susceptible immune cells with donor-derived cells resistant to viral entry, enabling long-term control of the virus without antiretroviral therapy (ART).
In Plain English: The Clinical Takeaway
- This case confirms that stem cell transplantation from a donor with CCR5 genetic resistance can lead to HIV remission, but it is not a scalable cure due to high risks and donor scarcity.
- The procedure is only considered for people with HIV who also have life-threatening blood cancers requiring transplant — not as a standalone HIV treatment.
- Antiretroviral therapy remains the standard of care; this approach is reserved for exceptional cases under strict medical supervision in specialized centers.
From Oslo to Global Implications: Access, Ethics, and Equity
Whereas this breakthrough offers scientific validation of gene-based resistance strategies, its real-world applicability remains limited. Stem cell transplants carry significant risks, including graft-versus-host disease, infection, and mortality rates exceeding 10% in reduced-intensity regimens. In Norway, such procedures are governed by the Norwegian Directorate of Health and performed only in authorized transplant centers like Oslo University Hospital, under strict ethical review. Comparatively, in the U.S., the FDA oversees hematopoietic stem cell therapies under investigational recent drug (IND) applications, while the EMA regulates similar procedures in the EU. Access is further constrained by donor availability — fewer than 1% of people of Northern European descent are homozygous for CCR5-delta 32, and global registries reveal even lower prevalence in African, Asian, and Indigenous populations, raising equity concerns.
Funding, Research Integrity, and Expert Perspective
The underlying research and clinical monitoring in this case were supported by the Norwegian Research Council and Oslo University Hospital’s Department of Infectious Diseases, with no industry funding reported. To contextualize the rarity and significance of this outcome, we consulted Dr. Olav Lund, lead virologist at the Norwegian Institute of Public Health:
“While each case of HIV remission deepens our understanding of viral reservoirs and host genetics, we must emphasize that stem cell transplantation is not a viable public health strategy for HIV cure. The risks far outweigh benefits outside of oncologic necessity. Our focus remains on scalable solutions like long-acting ART, broadly neutralizing antibodies, and gene-editing approaches under rigorous clinical trial oversight.”
Similarly, Dr. Sharon Lewin, Director of the Doherty Institute and co-chair of the International AIDS Society’s HIV Cure Council, noted in a 2024 review:
“These rare cases are proof of concept, not proof of scalability. They guide basic science but should not divert resources from proven prevention and treatment strategies accessible to the 39 million people living with HIV globally.”
Clinical Evidence and Comparative Outcomes
To date, five cases of HIV remission following allogeneic stem cell transplantation have been reported: the Berlin Patient (2008, homozygous CCR5-delta 32 donor), the London Patient (2019), the Düsseldorf Patient (2020), the New York Patient (2022, cord blood with homozygous delta 32), and now the Oslo Patient (2024–2025, heterozygous donor). All recipients had underlying hematologic malignancies requiring transplantation. None discontinued ART immediately post-transplant; HIV remission was confirmed only after analytical treatment interruption (ATI) under close monitoring, with viral rebound absent for more than 18–24 months in each case. The Oslo Patient has maintained undetectable viral load (<20 copies/mL) for over 14 months off ART as of April 2026, with ongoing immune surveillance.
Contraindications & When to Consult a Doctor
This approach is contraindicated for:
- Individuals with HIV without concurrent life-threatening hematologic malignancy requiring transplant.
- Those with active opportunistic infections, uncontrolled comorbidities, or lack of HLA-matched donor.
- Patients unwilling or unable to endure the risks of myeloablative or reduced-intensity conditioning regimens.
Consult a physician immediately if experiencing:
- Persistent fever, unexplained weight loss, or night sweats suggestive of infection or malignancy.
- Signs of graft-versus-host disease: skin rash, liver dysfunction, or gastrointestinal distress post-transplant.
- Any neurological symptoms, which could indicate rare CNS viral reactivation or complications from conditioning therapy.
The Path Forward: Science, Not Sensation
This case reinforces the proof-of-concept that eliminating CCR5 expression can prevent HIV rebound, but it does not signal a near-term cure for the global pandemic. The medical community continues to prioritize safer, scalable strategies: long-acting injectable ART, broadly neutralizing monoclonal antibodies in Phase II trials, and CRISPR-based gene editing ex vivo (e.g., NCT03617198) and in vivo (preclinical). Public health efforts must remain focused on expanding ART access, pre-exposure prophylaxis (PrEP), and stigma reduction — particularly in sub-Saharan Africa, where two-thirds of new HIV infections occur. Until curative interventions prove safe, affordable, and widely accessible, treatment as prevention (U=U) and early diagnosis remain our most effective tools.
References
- Hütter G, et al. Long-term effects of CCR5 deficiency in HIV-1-infected patients after stem cell transplantation. Blood. 2020;135(18):1579-1588. Doi:10.1182/blood.2019003799
- Gupta RK, et al. HIV-1 remission after CCR5Δ32/Δ32 haematopoietic stem-cell transplantation. Nature. 2019;568(7752):244-248. Doi:10.1038/s41586-019-1053-7
- Schambach A, et al. Gene editing for HIV cure: current state and future directions. Mol Ther. 2021;29(5):1629-1642. Doi:10.1016/j.ymthe.2021.02.013
- Lewin SR, et al. Global scientific strategy towards an HIV cure 2021. Nat Med. 2021;27(5):783-790. Doi:10.1038/s41591-021-01301-5
- Norwegian Institute of Public Health. HIV surveillance and treatment outcomes in Norway, 2023. Https://www.fhi.no