A daughter’s public outcry over her father’s Parkinson’s disease and lack of pension has ignited a broader conversation about the socioeconomic burden of neurodegenerative disorders, particularly how chronic illness intersects with labor rights, healthcare access, and social safety nets in aging populations. While the emotional core of the story centers on familial injustice, the underlying medical reality — Parkinson’s disease affecting nearly 10 million people globally — demands a clinically grounded examination of its progression, treatment limitations, and systemic failures in long-term care support.
The Clinical Reality of Parkinson’s: Beyond Motor Symptoms
Parkinson’s disease is a progressive neurodegenerative disorder primarily characterized by the loss of dopaminergic neurons in the substantia nigra, a region of the midbrain critical for motor control. This neuronal degeneration leads to the hallmark motor symptoms: bradykinesia (slowness of movement), resting tremor, rigidity, and postural instability. However, non-motor symptoms — including cognitive decline, depression, sleep disorders, and autonomic dysfunction — often precede motor signs by years and significantly impair quality of life. In the case described, the father’s difficulty walking in enclosed spaces may reflect freezing of gait, a debilitating phenomenon linked to disrupted neural circuits involving the pedunculopontine nucleus and frontal cortex, not merely muscle weakness or fatigue.
While the exact etiology remains multifactorial, involving genetic predispositions (e.g., LRRK2, GBA mutations) and environmental exposures (such as pesticides or industrial solvents), approximately 85–90% of cases are sporadic. Age is the strongest risk factor, with incidence rising sharply after 60. Globally, Parkinson’s prevalence has doubled in the past 25 years, driven by aging populations and increased longevity, prompting the World Health Organization to classify it as a growing public health priority.
In Plain English: The Clinical Takeaway
- Parkinson’s is not just a movement disorder — it affects cognition, mood, and autonomic functions, often years before tremors appear.
- While treatments like levodopa can manage symptoms, they do not gradual disease progression and may cause complications over time.
- Long-term care needs, including physical therapy and home support, are frequently underfunded, leaving families to bear the emotional and financial burden.
Treatment Landscape: Symptomatic Relief Without a Cure
Current pharmacological therapies aim to replenish or mimic dopamine. Levodopa, converted to dopamine in the brain, remains the gold standard for symptomatic relief, often combined with carbidopa to prevent peripheral breakdown. However, long-term use is associated with motor fluctuations and dyskinesias — involuntary, writhing movements — affecting up to 50% of patients after five years. Alternative agents include dopamine agonists (e.g., pramipexole), MAO-B inhibitors (e.g., selegiline), and anticholinergics, each with distinct side effect profiles requiring careful titration.

For advanced cases, deep brain stimulation (DBS) — a neurosurgical procedure implanting electrodes in the subthalamic nucleus or globus pallidus interna — can significantly reduce motor symptoms and medication dependence. However, DBS is invasive, costly, and contraindicated in patients with significant cognitive impairment or untreated psychiatric conditions. Access varies widely: while covered under Medicare in the U.S. And the NHS in the UK, out-of-pocket costs in low- and middle-income countries often render it inaccessible.
Importantly, no current therapy modifies the underlying neurodegenerative process. Numerous disease-modifying trials targeting alpha-synuclein aggregation, neuroinflammation, or mitochondrial dysfunction have failed in Phase II and III, underscoring the complexity of the pathology. As Dr. Tanya Simuni, Professor of Neurology at Northwestern University Feinberg School of Medicine, stated in a 2023 consensus review:
“We are excellent at managing symptoms, but we have yet to deliver a therapy that changes the course of Parkinson’s disease. That remains the central unmet require in neurology.”
Geo-Epidemiological Bridging: Healthcare Access and Social Protection
The daughter’s frustration over her father’s lack of pension highlights a critical gap between medical need and social protection. In countries with robust social safety nets — such as Germany, Sweden, or Canada — individuals with Parkinson’s may qualify for disability benefits, long-term care insurance, or home health aides through national programs. In contrast, in many Latin American and South Asian nations, pension systems are contributory and often exclude informal workers, leaving those who developed chronic illness mid-career without support.

In the U.S., the Social Security Disability Insurance (SSDI) program provides benefits to those unable to operate due to Parkinson’s, but approval requires stringent documentation of functional limitation, a process that can take months or years. The NHS in the UK offers Parkinson’s nurse specialists and multidisciplinary teams through its long-term conditions framework, yet workforce shortages and regional disparities limit consistent access. Meanwhile, the WHO’s Mental Health Gap Action Programme (mhGAP) includes neurological disorders in its scaling-up guide, advocating for integration of Parkinson’s care into primary health systems in low-resource settings — a goal still far from realization.
Epidemiological data from the Global Burden of Disease Study 2021 shows that age-standardized disability-adjusted life years (DALYs) due to Parkinson’s are highest in high-income regions, not because the disease is more prevalent, but because populations live longer and disability is more comprehensively measured. Yet, treatment access remains inequitable: a 2022 Lancet Neurology analysis found that over 75% of people with Parkinson’s in low-income countries receive no neurologist-led care.
Contraindications & When to Consult a Doctor
- Individuals with a history of hallucinations, severe hypotension, or psychotic disorders should avoid dopamine agonists due to risk of worsening neuropsychiatric symptoms.
- Sudden worsening of mobility, confusion, or signs of infection (e.g., fever, urinary urgency) in a Parkinson’s patient warrants immediate medical evaluation — these may indicate delirium, medication side effects, or pneumonia, a leading cause of mortality.
- Patients experiencing compulsive behaviors (e.g., gambling, hypersexuality) while on dopaminergic therapy should consult their neurologist, as these are known impulse control disorders linked to medication overstimulation.
The Hidden Toll: Caregiver Burden and Economic Impact
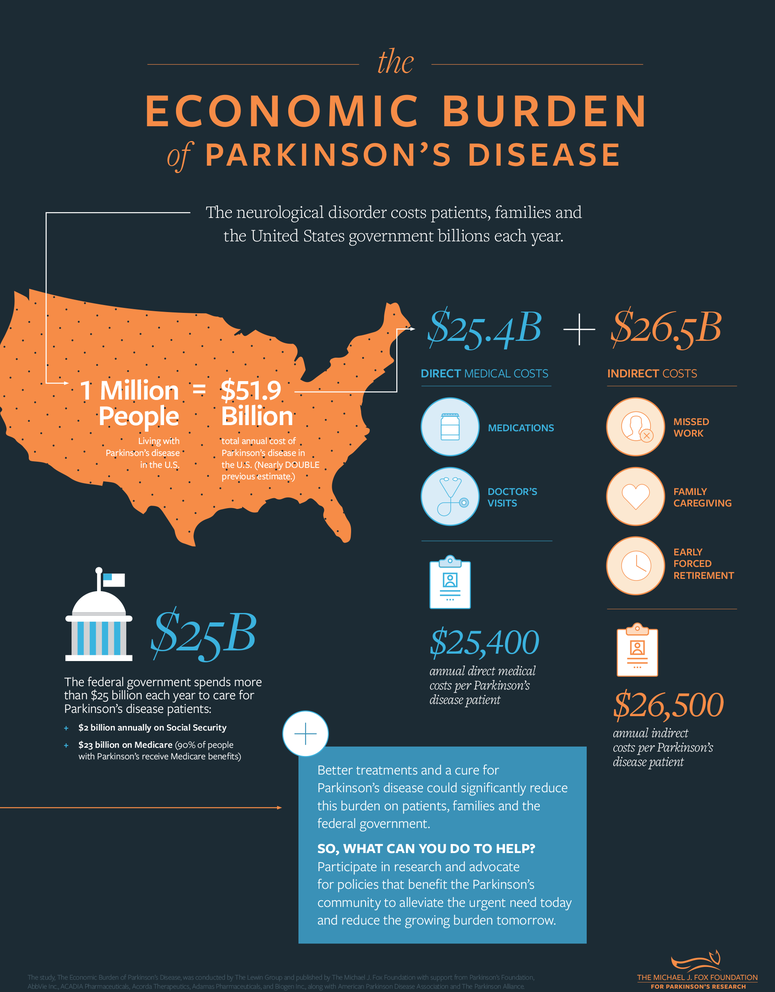
Beyond the patient, Parkinson’s imposes substantial strain on caregivers. A 2020 meta-analysis in Movement Disorders found that over 60% of family caregivers report clinically significant anxiety or depression, with financial strain being a key predictor. The indirect costs — lost wages, reduced productivity, and informal care — often exceed direct medical expenses. In Europe, the annual cost of Parkinson’s per patient is estimated at €10,000–€15,000, rising to over €25,000 in advanced stages due to nursing home placement.
This economic reality underscores why stories like the daughter’s resonate: they are not isolated incidents but symptoms of systemic failure to support aging workers who develop debilitating conditions. As Dr. Bastiaan Bloem, neurologist and Parkinson’s expert at Radboud University Medical Center, emphasized in a 2021 WHO interview:
“Parkinson’s is not just a medical condition — it’s a social emergency. We need policies that recognize chronic disability as a societal responsibility, not a family burden.”
Looking Ahead: Research, Equity, and the Need for Integrated Care
Emerging strategies include gene therapies targeting GBA or LRRK2 mutations, alpha-synuclein immunotherapies, and novel neuroprotective agents like ambroxol or UDCA, though none have yet demonstrated conclusive efficacy in slowing progression. Adaptive trial platforms, such as those pioneered by the Parkinson’s Progressive Markers Initiative (PPMI), aim to accelerate identification of disease-modifying treatments by enriching cohorts with biomarkers.
Equally vital is the push for integrated care models that combine neurology, rehabilitation, mental health, and social services. Programs like Parkinson’s Foundation’s Centers of Excellence or the European Parkinson’s Disease Association (EPDA) advocacy for national care standards represent steps toward systemic reform. Until such frameworks are universally accessible, stories of indignity will persist — not because science has failed, but because society has failed to match medical understanding with moral obligation.
References
- Simon DK, Tanner CM, Brundin P. Parkinson disease pathogenesis and treatment advances. Ann Neurol. 2020;88(4):639-656. Doi:10.1002/ana.25831
- Global Burden of Disease Collaborative Network. Global Burden of Disease Study 2021 (GBD 2021) Results. Seattle, United States: Institute for Health Metrics and Evaluation (IHME), 2022.
- Schrag A, et al. Cost of Parkinson’s disease in the UK: a prevalence-based study. J Neurol Neurosurg Psychiatry. 2001;70(5):618-624.
- Simuni T, et al. Disease modification in Parkinson’s disease: targeting alpha-synuclein. Mov Disord. 2020;35(1):15-29.
- Bloem BR, et al. Moving forward: Parkinson’s disease advocacy and policy. Lancet Neurol. 2021;20(4):259-261.

