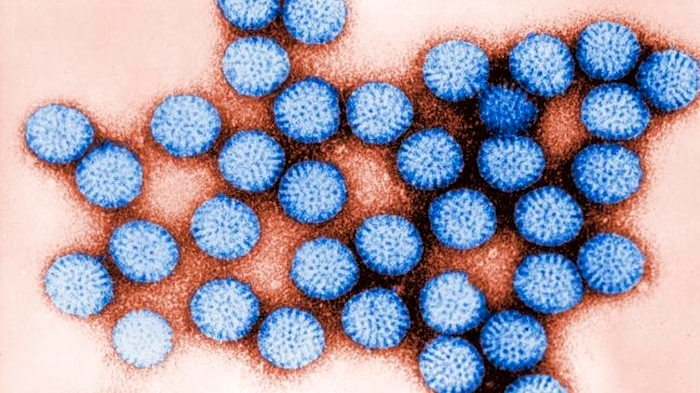
Rotavirus cases are rising in the United States, driven by seasonal patterns and localized gaps in immunization coverage, though the highly effective rotavirus vaccine continues to prevent approximately 80% of severe hospitalizations in vaccinated children, according to recent epidemiological data. The virus, a leading cause of dehydrating diarrhea in infants and young children, spreads primarily through the fecal-oral route, with outbreaks often peaking in winter and spring months. Public health officials emphasize that timely vaccination remains the most effective strategy to mitigate transmission and reduce strain on pediatric healthcare systems.
Understanding the Surge: Seasonal Trends and Immunity Gaps
Rotavirus infections follow a predictable seasonal pattern in temperate climates, typically increasing from January through June in the Northern Hemisphere. In 2024–2025, the CDC reported a 22% rise in laboratory-confirmed rotavirus cases compared to the previous season, particularly in regions with suboptimal vaccine uptake, including parts of the Northeast and Midwest. While national immunization rates for the rotavirus vaccine series remain above 70%, pockets of under-vaccination persist due to access barriers, vaccine hesitancy, and disruptions in routine pediatric care during and after the pandemic.
The virus is highly contagious, with as few as 100 viral particles capable of causing infection. It infects mature enterocytes on the villi of the compact intestine, where it replicates and disrupts nutrient and fluid absorption, leading to watery diarrhea, vomiting, fever, and abdominal pain. In severe cases, dehydration can develop rapidly, necessitating intravenous rehydration and hospitalization—especially in infants under two years of age.
In Plain English: The Clinical Takeaway
- Rotavirus spreads easily through contaminated hands, surfaces, or objects—frequent handwashing with soap and water is critical, as alcohol-based sanitizers are less effective against this non-enveloped virus.
- The rotavirus vaccine (administered orally at 2, 4, and sometimes 6 months of age) prevents severe disease in about 90% of recipients and reduces hospitalizations by up to 80%, based on over a decade of real-world data.
- Even vaccinated children may experience mild, asymptomatic infection, but they are far less likely to develop dangerous dehydration requiring medical intervention.
Geo-Epidemiological Bridging: Vaccine Access and Public Health Response
In the United States, the Advisory Committee on Immunization Practices (ACIP) recommends routine rotavirus vaccination for all infants, with the first dose administered by 15 weeks of age and the series completed by 8 months. Two live-attenuated oral vaccines are licensed: Rotarix® (GSK) and RotaTeq® (Merck). Both have undergone rigorous Phase III clinical trials involving over 70,000 infants collectively, demonstrating strong efficacy against severe rotavirus gastroenteritis and an acceptable safety profile, with no increased risk of intussusception beyond background levels in large post-licensure studies.
Funding for pivotal trials came from a combination of public-private partnerships: the Rotarix® pivotal trial was supported by GlaxoSmithKline Biologicals, while the RotaTeq® trials were funded by Merck & Co., with independent data monitoring committees overseeing safety outcomes. The CDC’s Vaccines for Children (VFC) program ensures free vaccine access for uninsured or underinsured children, helping to reduce disparities in protection.
In Europe, the European Medicines Agency (EMA) has authorized both vaccines, and national immunization programs in countries like the UK, Germany, and Italy report similar reductions in rotavirus hospitalizations—often exceeding 70%—following vaccine introduction. The NHS in England introduced Rotarix® into its routine schedule in 2013, resulting in a sustained decline in seasonal burden.
“Vaccination doesn’t just protect the individual child—it creates community-level immunity that interrupts transmission chains, especially in settings like daycare centers where rotavirus spreads rapidly.” — Dr. Umesh Parashar, Lead Epidemiologist, Viral Gastroenteritis Team, CDC Division of Viral Diseases, personal communication, April 2025.
“We’ve seen consistent evidence that high vaccine coverage not only prevents severe disease but also reduces the overall circulation of rotavirus in the population, offering indirect protection to unvaccinated infants too young to be immunized.” — Dr. Margaret Rennels, Professor of Pediatrics, University of Maryland School of Medicine, former chair of the ACIP Rotavirus Working Group, Journal of the Pediatric Infectious Diseases Society, 2024.
Mechanism of Action and Immune Response
Rotaviruses are double-stranded RNA viruses classified under the Reoviridae family. They infect host cells by binding to specific glycans on the intestinal epithelium via their VP4 spike protein, followed by VP7-mediated membrane fusion. Once inside, the virus uses the cell’s machinery to replicate its genome and produce new viral particles, which are shed in high concentrations in stool—often exceeding 1012 viral particles per gram during peak infection.
The oral rotavirus vaccines operate by introducing weakened strains that replicate minimally in the gut, triggering a local IgA immune response in the intestinal mucosa—the primary defense against reinfection. This mucosal immunity, combined with systemic antibody responses, provides durable protection against severe disease. Unlike injectable vaccines, oral rotavirus vaccines do not require needles, improving acceptability and ease of administration in resource-limited settings.
Contraindications & When to Consult a Doctor
The rotavirus vaccine is contraindicated in infants with a history of severe combined immunodeficiency (SCID), as live vaccines pose a risk of uncontrolled replication in severely immunocompromised individuals. It should also be avoided in those with a history of intussusception, a rare bowel obstruction, although current evidence shows the risk of vaccine-associated intussusception is low—approximately 1 to 5 additional cases per 100,000 vaccinated infants—and is far outweighed by the benefits of preventing severe dehydrating diarrhea.
Parents should seek immediate medical attention if a child shows signs of dehydration: dry mouth, absence of tears when crying, decreased urine output (fewer than six wet diapers per day in infants), sunken eyes, lethargy, or irritability. Persistent vomiting, high fever (>102°F or 38.9°C), or bloody stool also warrant prompt evaluation, as these may indicate complications or alternative diagnoses such as bacterial enteritis.
For mild cases, oral rehydration solutions (ORS) containing precise ratios of glucose and electrolytes are recommended over plain water or sugary drinks, which can worsen diarrhea. The WHO and CDC endorse ORS as the first-line treatment for mild to moderate dehydration from gastroenteritis in children.
Looking Ahead: Sustaining Gains in Vaccine Confidence
Despite the proven success of rotavirus vaccines, maintaining high coverage requires ongoing public health outreach, provider education, and efforts to counter misinformation. A 2023 study in Vaccine found that parental concerns about vaccine safety—often amplified on social media—remained a key driver of delay or refusal, even when efficacy was well understood. Addressing these concerns with transparent, empathetic communication is essential to prevent backsliding in disease control.
Surveillance systems like the CDC’s New Vaccine Surveillance Network (NVSN) continue to monitor rotavirus genotypes and vaccine effectiveness in real time, ensuring that circulating strains remain covered by existing vaccines. To date, no significant antigenic drift has necessitated vaccine reformulation, a testament to the stability of the VP7 and VP4 proteins targeted by current immunogens.
As seasonal increases continue, the message remains clear: vaccination is not just a personal health decision—This proves a public health safeguard. By ensuring timely immunization, practicing diligent hygiene, and recognizing early signs of dehydration, families and clinicians can work together to keep rotavirus from becoming a preventable burden on children’s health.
References
- Parashar UD, et al. Global Impact of Rotavirus Vaccination on Childhood Hospitalizations and Mortality. Journal of Infectious Diseases. 2020;221(Suppl 4):S336-S344.
- Richardson V, et al. Effectiveness of Monovalent Rotavirus Vaccine (Rotarix) Against Severe Diarrhea in US Infants. Pediatrics. 2010;125(5):e1064-e1071.
- Velázquez FR, et al. Efficacy and Safety of an Oral Live Attenuated Human Rotavirus Vaccine. The New England Journal of Medicine. 2006;354(1):11-22.
- Clark HF, et al. Evaluation of Pentavalent Human-Bovine (WC3) Reassortant Rotavirus Vaccine in Healthy Infants. The New England Journal of Medicine. 2004;350(1):32-39.
- Tate JE, et al. Global Impact of Rotavirus Vaccine Introduction on Childhood Hospitalizations and Mortality. The Lancet Global Health. 2016;4(7):e465-e472.