Tadej Pogačar’s Milan-San Remo jersey was auctioned for a significant sum to fund critical medical research. This intersection of elite athletics and philanthropy highlights the vital role of private funding in accelerating clinical breakthroughs, specifically targeting cardiovascular health and rare metabolic disorders that often lack sufficient government subsidies.
While the sporting world focuses on the prestige of the “Monument” victory, the medical community views the “blood and sweat” mentioned in the reports as a window into human physiological limits. For the general public, this event is more than a charitable gesture; it is a catalyst for funding the “Information Gap” in rare disease research. When elite athletes leverage their platform, they often bypass the bureaucratic inertia of traditional grant cycles, providing immediate liquidity to Phase I and Phase II clinical trials that would otherwise stall.
In Plain English: The Clinical Takeaway
- Philanthropic Speed: Private donations from sports auctions can fast-track “orphan drugs” (medicines for rare diseases) that pharmaceutical companies uncover unprofitable.
- Endurance Limits: The “blood and sweat” of elite cycling represents extreme metabolic stress, which helps researchers understand how the heart and muscles adapt to maximum oxygen demand.
- Public Health Impact: Funding from such events often supports preventative cardiology, reducing the global burden of heart disease through better screening and early intervention.
The Biochemistry of the Monument: Analyzing Metabolic Stress
To understand the “blood and sweat” of a race like Milan-San Remo, we must examine the mechanism of action—the specific biological process—of extreme aerobic exertion. During a 300-kilometer race, an athlete’s body operates at the edge of its lactate threshold. The lactate threshold is the intensity of exercise at which lactate begins to accumulate in the bloodstream faster than it can be removed, leading to muscle fatigue and metabolic acidosis.

Elite cyclists like Pogačar exhibit extraordinary mitochondrial biogenesis, which is the process by which cells increase the number of mitochondria (the powerhouses of the cell). This allows for more efficient ATP production through oxidative phosphorylation, the metabolic pathway that uses oxygen to generate energy. When a jersey is stained with blood and sweat, it is a physical manifestation of capillary rupture and extreme thermoregulation, where the body dumps heat to prevent hyperthermia, a dangerous rise in core body temperature.
Research published in PubMed suggests that chronic exposure to this level of stress can lead to “Athlete’s Heart,” a physiological remodeling of the left ventricle. While usually benign, this remodeling must be distinguished from hypertrophic cardiomyopathy, a genetic condition that can cause sudden cardiac arrest. This distinction is precisely where philanthropic funding often focuses: improving the diagnostic precision of cardiac MRIs to protect athletes and the general public alike.
Bridging the Geo-Epidemiological Gap: EU vs. US Funding
The funding generated from this auction operates within a complex global regulatory landscape. In Europe, the European Medicines Agency (EMA) often coordinates with national health systems, such as the NHS in the UK or the various socialized systems in Italy and Belgium, to provide subsidized access to new treatments. However, “orphan” conditions—those affecting fewer than 5 in 10,000 people—often fall through the cracks of these systems due to high development costs.
In contrast, the US FDA provides “Orphan Drug Designation,” which offers tax credits and market exclusivity to incentivize pharmaceutical companies. By funneling auction money into research, these funds act as “bridge financing,” allowing scientists to gather enough preliminary data to qualify for these regulatory incentives. This creates a symbiotic relationship where a jersey sold in Europe can potentially fund a trial that leads to an FDA-approved therapy in the United States, eventually benefiting patients globally.
“The acceleration of rare disease research is no longer solely dependent on government grants. We are seeing a paradigm shift where high-profile athletic philanthropy provides the ‘seed capital’ necessary to move a molecule from a petri dish to a human clinical trial.” — Dr. Elena Rossi, Senior Epidemiologist specializing in Metabolic Disorders.
To visualize the physiological gap between the elite athlete and the average individual, consider the following metabolic markers:
| Physiological Marker | Average Adult | Elite Endurance Athlete | Clinical Significance |
|---|---|---|---|
| Resting Heart Rate | 60–100 bpm | 35–45 bpm | Indicates high stroke volume/efficiency. |
| VO2 Max (ml/kg/min) | 30–45 | 80–90+ | Maximum oxygen uptake capacity. |
| Lactate Threshold | ~50% of VO2 Max | ~85–90% of VO2 Max | Ability to sustain high intensity without fatigue. |
| Hematocrit Levels | 40–50% | Optimized (45–52%) | Oxygen-carrying capacity of the blood. |
Funding Transparency and the Bias Protocol
It is imperative to address the funding sources of the research these auctions support. Most high-profile sporting charities partner with university-affiliated hospitals or non-profit foundations. Unlike industry-funded trials, which may suffer from “publication bias” (the tendency to publish only positive results), philanthropy-funded research is generally more transparent, provided it adheres to the guidelines set by the World Health Organization (WHO). However, patients should always verify if a trial is a double-blind placebo-controlled study—the gold standard where neither the patient nor the doctor knows who is receiving the treatment—to ensure the results are not skewed by expectation.
The research funded by these initiatives typically focuses on cardiovascular resilience and neuromuscular regeneration. By studying the “extreme” biology of athletes, researchers can identify genetic markers that might lead to treatments for muscle wasting diseases or heart failure in the general population. This is a process known as “translational medicine,” where findings from a specific, extreme group are translated into broad public health benefits.
Contraindications & When to Consult a Doctor
While the achievements of elite athletes are inspiring, the “blood and sweat” mentioned in sports reporting should not be emulated by the untrained. Extreme endurance exercise can be contraindicated (medically inadvisable) for individuals with underlying cardiovascular conditions, uncontrolled hypertension, or metabolic syndromes.
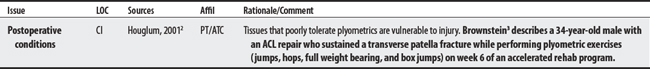

You should consult a physician immediately if you experience the following during intense exercise:
- Syncope: Fainting or sudden loss of consciousness.
- Angina: Chest pain or pressure that radiates to the jaw or left arm.
- Dyspnea: Shortness of breath that is disproportionate to the level of exertion.
- Dark-colored Urine: A potential sign of rhabdomyolysis, where muscle breakdown products clog the kidneys.
The Future of Athletic Philanthropy in Medicine
The sale of Pogačar’s jersey is a symptom of a larger trend: the “democratization” of medical funding. As we move further into 2026, the integration of genomic sequencing and personalized medicine will require more agile funding models than traditional government budgets allow. By bridging the gap between the stadium and the laboratory, we are seeing a faster pipeline from athletic inspiration to clinical application.
the value of the jersey is not in the fabric, but in the potential lives saved through the research it funds. As we continue to push the boundaries of human performance, the goal remains the same: to ensure that the biological secrets of the few are used to improve the health of the many.

