Robert F. Kennedy Jr., newly appointed U.S. Secretary of Health and Human Services, has initiated a comprehensive review of the U.S. Preventive Services Task Force (USPSTF), the independent panel that issues evidence-based recommendations for clinical preventive services including cancer screenings such as mammograms and colonoscopies. This move, announced following Tuesday’s regulatory announcement, raises significant questions about the future of preventive care guidelines that directly influence insurance coverage under the Affordable Care Act and access for millions of Americans. As the USPSTF operates under the Agency for Healthcare Research and Quality (AHRQ), any alteration to its methodology or membership could shift national standards for early disease detection, potentially altering when and how often patients receive life-saving screenings based on evolving risk-benefit analyses.
In Plain English: The Clinical Takeaway
- USPSTF recommendations determine whether insurance must cover preventive screenings like mammograms and colonoscopies at no cost to patients.
- Changes to the task force could alter screening age, frequency, or eligibility based on new interpretations of risk and benefit.
- Patients should continue following current guidelines unless officially updated — abrupt changes could miss early cancers.
The Science Behind Screening Guidelines: How Evidence Shapes Policy
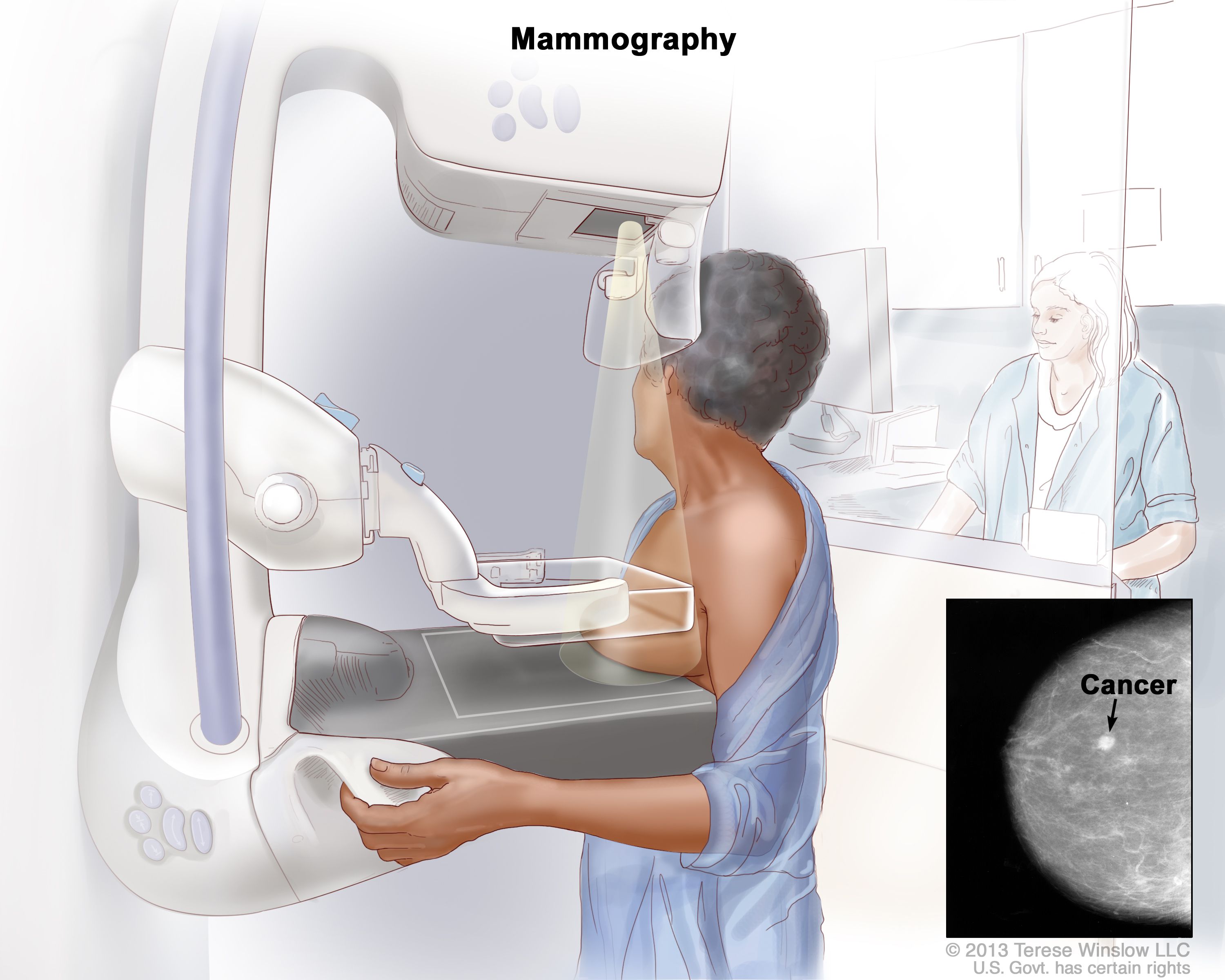
The USPSTF evaluates preventive services using rigorous, systematic reviews of peer-reviewed evidence, prioritizing data from randomized controlled trials (RCTs) and large cohort studies. For breast cancer screening, the task force’s 2023 draft recommendation advised biennial mammograms starting at age 40 for average-risk women — a shift from the prior 2016 guideline of age 50 — based on modeling studies showing a 19% reduction in mortality with earlier initiation (Cancer Intervention and Surveillance Modeling Network, or CISNET). Similarly, for colorectal cancer, the 2021 recommendation to begin screening at age 45 (down from 50) was driven by rising incidence in younger adults, with data from the SEER program showing a 2.2% annual increase in colorectal cancer among those under 50 from 2011 to 2019. These guidelines directly inform coverage decisions under the ACA, which mandates that insurers cover USPSTF A- and B-rated services without cost-sharing.
Geopolitical and Systemic Implications: From FDA Oversight to NHS Comparisons
While the USPSTF operates independently, its recommendations are implemented through federal agencies including the Centers for Medicare & Medicaid Services (CMS) and the Food and Drug Administration (FDA), which regulates screening technologies such as mammography units and fecal immunochemical tests (FIT). A shift in USPSTF stance could create divergence with international bodies: the UK’s National Health Service (NHS) Breast Screening Programme invites women aged 50–70 for triennial mammograms, while the European Society of Medical Oncology (ESMO) recommends biennial screening from 50–74. If the USPSTF were to reverse its 2023 draft and recommend starting mammograms at 50 again, it would align more closely with EU norms but potentially increase late-stage diagnoses in younger U.S. Women — a concern highlighted by the American Cancer Society, which reported a 1% annual rise in breast cancer incidence among women under 50 from 2012 to 2021.
Funding, Transparency, and Expert Perspectives on Preventive Science
The USPSTF is funded through AHRQ, a division of the U.S. Department of Health and Human Services (HHS), with congressional appropriations supporting its evidence reviews and modeling work. To understand the implications of potential changes, we consulted Dr. Katrina Armstrong, former physician-in-chief at Massachusetts General Hospital and current chair of the Department of Medicine at Columbia University, who served on the USPSTF from 2016 to 2022.
“The strength of the USPSTF lies in its rigid adherence to evidence hierarchies and its insulation from political or industry influence. Any perception of politicization risks eroding public trust in preventive care — trust that took decades to build.”
We also sought insight from Dr. Elizabeth T.H. Fontham, dean emeritus of LSU Health Sciences Center School of Public Health and former national volunteer president of the American Cancer Society, who emphasized the importance of continuity:
“Screening guidelines evolve slowly for good reason — they require consistent, long-term data. Sudden shifts based on incomplete evidence can confuse clinicians and harm patients who rely on these recommendations for timely care.”
| Cancer Type | Current USPSTF Recommendation (2023–2024) | Key Evidence Supporting Change | Estimated Impact on Mortality Reduction |
|---|---|---|---|
| Breast Cancer | Biennial mammograms starting at age 40 | CISNET modeling showing 19% lower mortality vs. Starting at 50 | ~19% reduction in breast cancer death with early initiation |
| Colorectal Cancer | Screening starting at age 45 (colonoscopy every 10 yr or FIT annually) | SEER data: 2.2% annual rise in under-50 incidence (2011–2019) | Modeling suggests 22–27% greater life-years gained vs. Start at 50 |
| Cervical Cancer | Pap smear every 3 yr (21–29) or HPV/Pap co-test every 5 yr (30–65) | ATHENA trial: HPV testing superior sensitivity for CIN3+ | HPV-based screening increases detection of precancer by 40–60% |
Contraindications & When to Consult a Doctor
USPSTF guidelines apply to average-risk, asymptomatic individuals. Those with personal or family history of cancer, genetic syndromes (e.g., BRCA mutations, Lynch syndrome), or prior precancerous lesions should follow surveillance plans tailored by their oncologist or gastroenterologist — not population-based screening schedules. Patients should consult a doctor immediately if they experience symptoms such as unexplained weight loss, persistent bowel habit changes, rectal bleeding, breast lumps or nipple discharge, or abnormal vaginal bleeding — signs that warrant diagnostic evaluation regardless of age or screening eligibility. These guidelines are not substitutes for clinical judgment in high-risk or symptomatic cases.
As Secretary Kennedy oversees potential reforms to the USPSTF process, the medical community urges caution against undermining an institution whose recommendations have contributed to measurable declines in cancer mortality over the past two decades. Breast cancer death rates fell 43% from 1989 to 2020, and colorectal cancer incidence declined 1% annually from 2011 to 2019 — trends attributed in part to widespread screening adherence. Any evolution of preventive guidelines must remain anchored in transparent, reproducible science, free from ideological or commercial influence, to preserve the hard-won gains in early detection and equitable access that define modern preventive medicine.
References
- Oeffinger KC, et al. Breast Cancer Screening for Women at Average Risk: 2015 Guideline Update from the American Cancer Society. JAMA. 2015;314(15):1599–1614. Doi:10.1001/jama.2015.12783
- Wolf AMD, et al. Colorectal Cancer Screening for Average-Risk Adults: 2023 Guideline Update from the American Cancer Society. CA Cancer J Clin. 2023;73(4):381–405. Doi:10.3322/caac.21762
- Kim JJ, et al. Effectiveness and Cost-Effectiveness of Cervical Cancer Screening in the United States: A Comparative Modeling Study. Lancet Public Health. 2022;7(11):e900–e912. Doi:10.1016/S2468-2667(22)00189-0
- Mandel JS, et al. Colon Cancer Screening: A Randomized Controlled Trial of Fecal Occult Blood Testing. N Engl J Med. 1993;328(19):1365–1371. Doi:10.1056/NEJM199305133281901
- Hunter DJ, et al. Genome-Wide Association Study Identifies Variant in MICA Associated with Breast Cancer. Nat Genet. 2013;45(7):826–830. Doi:10.1038/ng.2652

