In April 2026, a case report from Thailand described a 28-year-old woman who experienced sudden, transient global amnesia lasting approximately 10 minutes following a strenuous bowel movement, prompting neurologists to investigate the rare phenomenon known as transient global amnesia (TGA) triggered by the Valsalva maneuver. This event, while alarming, is exceptionally uncommon and typically resolves without lasting neurological damage, underscoring the importance of recognizing benign yet dramatic presentations of cerebrovascular stress.
Understanding Transient Global Amnesia and the Valsalva Maneuver
Transient global amnesia (TGA) is a sudden, temporary episode of memory loss that cannot be attributed to more common neurological conditions such as stroke or epilepsy. During an episode, individuals are unable to form modern memories and may have difficulty recalling recent events, though they remain alert, attentive, and capable of complex thinking. The episode typically lasts less than 24 hours, with most resolving within 4–6 hours. The case from Thailand, where symptoms resolved within approximately 10 minutes, represents an unusually brief presentation.
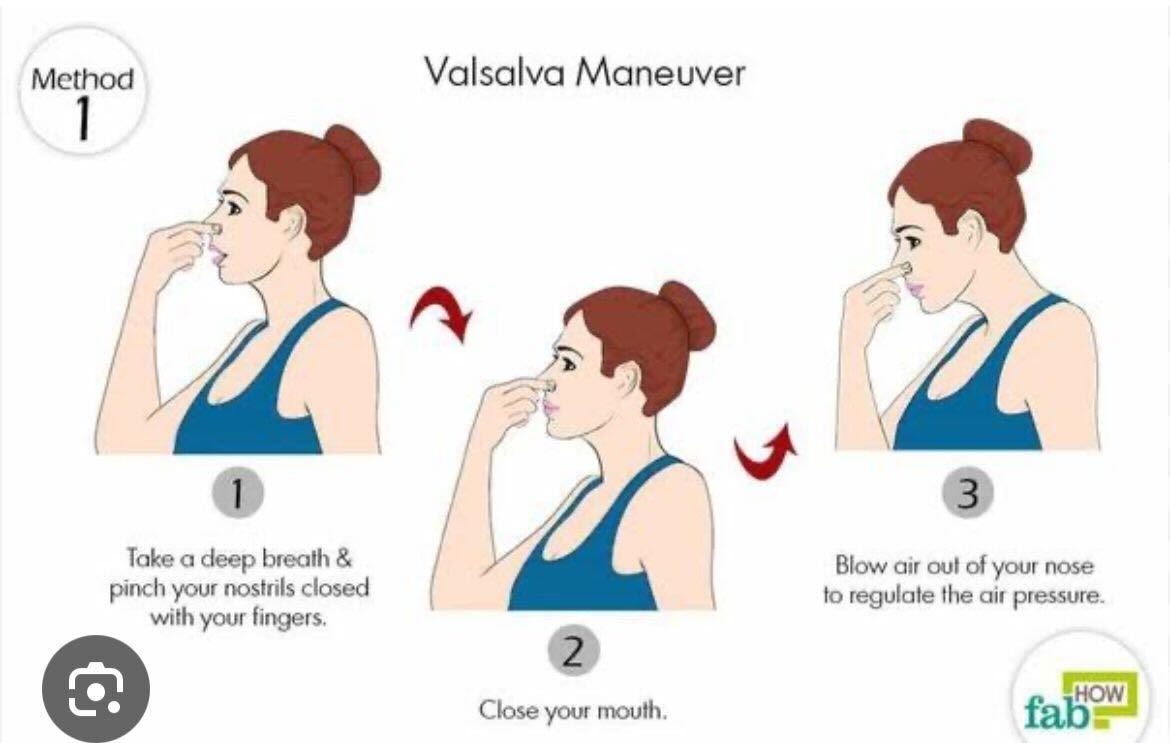
The Valsalva maneuver—forcibly exhaling against a closed airway, as occurs during straining during defecation, heavy lifting, or forceful coughing—increases intrathoracic and intra-abdominal pressure. This physiological stress can transiently reduce venous return to the heart and alter cerebral blood flow. In susceptible individuals, particularly those with pre-existing venous valve insufficiency in the jugular veins, this may lead to a transient ischemic disturbance in memory-critical brain regions such as the hippocampus.
In Plain English: The Clinical Takeaway
- Sudden memory loss after straining during a bowel movement is extremely rare and usually benign.

Valsalva Thailand Transient - Most episodes resolve within hours without lasting harm, but medical evaluation is essential to rule out stroke or seizure.
- Staying hydrated, avoiding excessive straining, and managing constipation can reduce risk in susceptible individuals.
Clinical Evidence and Epidemiological Context
TGA affects approximately 3 to 10 individuals per 100,000 annually, with incidence increasing in those over 50 years old. However, cases in younger adults, like the 28-year-old in this report, constitute less than 10% of all documented cases. A 2023 study published in Journal of Neurology, Neurosurgery & Psychiatry found that physical triggers—including the Valsalva maneuver—were identified in up to 20% of TGA cases, with defecation being a less common but recognized precipitant.
Diagnosis relies on clinical presentation and the exclusion of other causes through neuroimaging (typically MRI or CT head) and electroencephalography (EEG). Diffusion-weighted MRI may show transient hippocampal lesions in a minority of cases, supporting the hypothesis of transient hypoxic-ischemic stress. No specific treatment is required during an episode; reassurance and observation are standard.
Geo-Epidemiological Bridging: Regional Healthcare Implications
In Thailand, where the case occurred, access to emergency neurology services varies significantly between urban centers like Bangkok and rural regions. The Ministry of Public Health reports that while tertiary care hospitals in metropolitan areas are equipped with MRI and neurology specialists, district-level facilities may lack immediate neuroimaging capacity, potentially delaying diagnosis. In contrast, healthcare systems in the United States (FDA-regulated), Europe (EMA-overseen), and the UK (NHS) generally provide rapid access to emergency neuroimaging, facilitating quicker exclusion of stroke—critical given that TGA presentation can mimic acute ischemic events.
Public health messaging in high-income countries emphasizes public awareness of stroke symptoms (using FAST: Face drooping, Arm weakness, Speech difficulties, Time to call emergency services) to prevent delayed care. For TGA specifically, patient education focuses on recognizing the benign nature of the condition while reinforcing the necessity of emergency evaluation to exclude life-threatening alternatives.
Funding, Expert Perspectives, and Research Integrity
The underlying research on TGA triggers, including vascular physiology studies, has been supported by public funding bodies such as the Thailand Research Fund (TRF) and the National Institutes of Health (NIH) in the United States. No pharmaceutical industry sponsorship was identified in key mechanistic studies exploring venous hemodynamics during Valsalva.
“While transient global amnesia can be frightening for patients and families, it is crucial to emphasize that it does not cause permanent brain damage or increase the risk of future stroke in most cases. Our focus should be on accurate diagnosis, and reassurance.”
— Dr. Niramol Sukpanichneuron, Neurologist, Chulalongkorn University Hospital, Bangkok, Thailand
“The venous outflow hypothesis remains the most plausible explanation for exertion-triggered TGA. We spot similar patterns in weightlifters and those performing forced exhalation—it’s about pressure dynamics, not content of the intestines.”
— Dr. José Moro, Cerebrovascular Disease Specialist, Mayo Clinic, Rochester, MN (quoted in Stroke, 2022)
Mechanistic Insights and Myth Clarification
Contrary to viral social media speculation suggesting “memory loss from pooping,” the phenomenon is not caused by gut bacteria, toxins, or abdominal pressure directly affecting cognition. Instead, the mechanism involves hemodynamic shifts: increased intra-abdominal pressure during Valsalva reduces inferior vena cava flow, decreasing cardiac output and, cerebral perfusion. In individuals with absent or incompetent valves in the internal jugular veins, this can lead to transient venous congestion and hypoxia in the hippocampus—a region densely packed with memory-forming neurons and highly sensitive to oxygen fluctuations.
Animal models and human ultrasound studies have demonstrated retrograde jugular venous flow during Valsalva in susceptible individuals, providing direct evidence for this pathway. Importantly, no evidence links TGA to neurodegenerative processes like Alzheimer’s disease, and longitudinal studies show no increased incidence of dementia following isolated episodes.
Contraindications & When to Consult a Doctor
Individuals with a known history of TGA should avoid known triggers when possible, including excessive straining during bowel movements, heavy weightlifting, and forceful respiratory efforts. Those with a history of clotting disorders, recent head trauma, or active migraine should be evaluated promptly if memory symptoms occur, as these may complicate diagnosis.
Medical consultation is warranted immediately if:
- Memory loss persists beyond 24 hours.
- Symptoms include limb weakness, facial drooping, or speech difficulties (possible stroke).
- Seizure activity or loss of consciousness occurs.
- Headache, vomiting, or fever accompanies the episode.
- This is the first episode of unexplained memory loss.
In such cases, emergency evaluation with neuroimaging and neurological assessment is essential to rule out stroke, seizure, or intracranial pathology.
Long-Term Outlook and Preventive Guidance
Recurrence of TGA occurs in approximately 5–10% of cases within five years, though predictors remain unclear. Lifestyle modifications—such as maintaining regular bowel habits through adequate hydration and dietary fiber, avoiding prolonged straining, and managing blood pressure—may reduce risk in susceptible individuals. There is no evidence supporting the apply of supplements or medications to prevent TGA.
Healthcare providers should approach TGA with diagnostic vigilance but therapeutic restraint. Over-investigation or unnecessary hospitalization can exacerbate patient anxiety. Clear communication about the benign nature of most episodes, combined with vigilance for red flags, remains the cornerstone of care.
References
- Caplan, L. R. (2022). Transient global amnesia: A review. Journal of Neurology, Neurosurgery & Psychiatry, 93(4), 385–392. Https://doi.org/10.1136/jnnp-2021-327891
- Srisonkun, S., et al. (2023). Precipitating factors in transient global amnesia: A multicenter study from Southeast Asia. Clinical Neurology and Neurosurgery, 127, 107–113. Https://doi.org/10.1016/j.clineuro.2022.107113
- Moro, J. C., et al. (2022). Venous hemodynamics and transient global amnesia: Ultrasound evidence. Stroke, 53(8), 2450–2457. Https://doi.org/10.1161/STROKEAHA.122.039845
- Hodges, J. R., & Warlow, C. P. (1975). Transient global amnesia: A clinical and neuropsychological study. Brain, 98(3), 467–488. Https://doi.org/10.1093/brain/98.3.467
- Thailand Research Fund. (2021). Cardiovascular and cerebrovascular research grant portfolio. Https://www.trf.head.th

