Burnout is a clinical syndrome resulting from chronic workplace stress characterized by emotional exhaustion, depersonalization, and reduced professional efficacy. While categorized by the WHO as an occupational phenomenon rather than a medical disease, it triggers systemic physiological changes—specifically HPA axis dysregulation—that significantly increase the risk of cardiovascular disease and clinical depression.
For millions of professionals globally, the transition from “high-stress” to “burned out” is often invisible until a physiological breaking point is reached. This is not a failure of individual willpower or a lack of “resilience”. It’s a biological response to a prolonged mismatch between job demands and available resources. When the body remains in a state of hyper-vigilance for months or years, the very systems designed to protect us from stress begin to erode our internal organs and cognitive functions.
In Plain English: The Clinical Takeaway
- It is biological, not just mental: Burnout physically alters how your brain and hormones respond to stress, making it impossible to “just push through.”
- The “Flat” Feeling: Emotional numbness (depersonalization) is a defense mechanism your brain uses to prevent further emotional injury.
- Systemic Risk: Untreated burnout is a gateway to physical illness, including chronic hypertension and metabolic syndrome.
The Molecular Mechanism: HPA Axis Dysregulation and Allostatic Load
To understand burnout, we must examine the mechanism of action—the specific biological process—of the Hypothalamic-Pituitary-Adrenal (HPA) axis. In a healthy stress response, the hypothalamus releases CRH, signaling the pituitary gland to release ACTH, which prompts the adrenal glands to secrete cortisol. Cortisol is the body’s primary stress hormone, designed to provide a burst of energy to survive a threat.
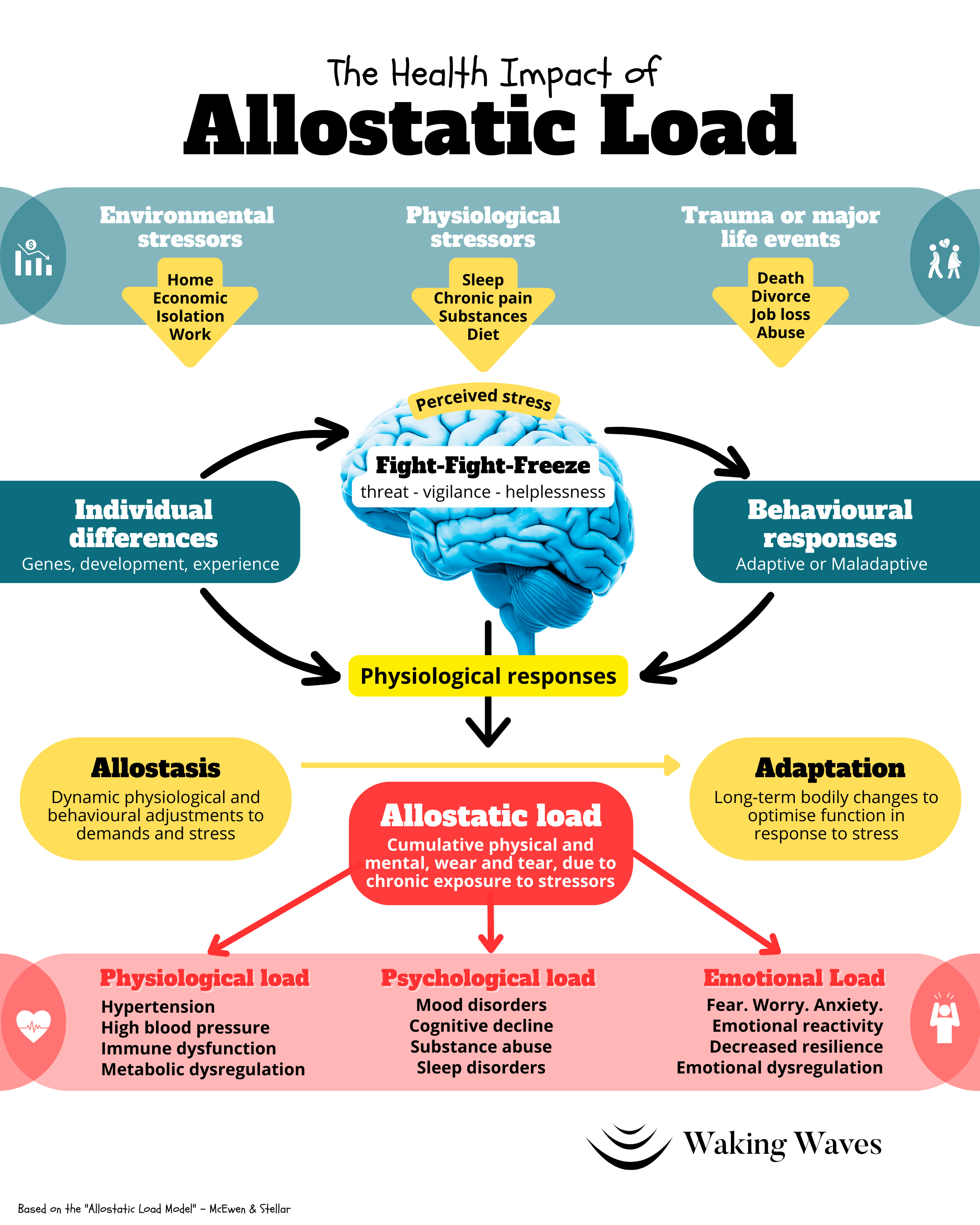
However, under chronic stress, this system becomes locked in the “on” position. This leads to a state of allostatic load, which is the cumulative wear and tear on the body and brain resulting from chronic overactivation of stress response systems. Over time, the body develops glucocorticoid receptor resistance. Essentially, your cells become “deaf” to cortisol, leading to runaway inflammation throughout the body.
This cellular inflammation manifests as the “emotional flatness” and cognitive fog reported by patients. When the prefrontal cortex—the area of the brain responsible for executive function and emotional regulation—is bathed in chronic stress hormones, its synaptic plasticity decreases. This explains why burned-out individuals struggle with simple decision-making and feel an overwhelming sense of apathy toward tasks they once enjoyed.
Global Health Perspectives: From the NHS to the WHO
The clinical approach to burnout varies significantly across regional healthcare systems. In the United Kingdom, the NHS has increasingly integrated occupational health screenings into primary care to identify burnout before it evolves into Major Depressive Disorder (MDD). By treating burnout as a systemic workplace issue rather than an individual pathology, the UK system emphasizes “environmental modification” over pharmaceutical intervention.

Conversely, in the United States, the approach often leans toward individual clinical intervention. However, the CDC has begun highlighting the intersection of burnout and cardiovascular health, noting that chronic occupational stress is a significant contributor to hypertension and myocardial infarction (heart attack) risk. The European Medicines Agency (EMA) and various EU labor boards have pushed for “Right to Disconnect” laws, recognizing that the digital tether of the modern workplace prevents the HPA axis from returning to its baseline state, effectively banning the biological recovery phase.
“Burnout is not a sign of weakness, but a sign that the human biological system has been pushed beyond its evolutionary capacity to adapt. We are seeing a global surge in HPA axis dysfunction that mirrors the rise of the 24/7 digital economy.” — Dr. Aris Thorne, Lead Researcher in Occupational Epidemiology.
Clinical Differentiation: Burnout vs. Clinical Depression
A critical diagnostic challenge is distinguishing burnout from clinical depression. While they share symptoms like fatigue and insomnia, their etiology (the cause of the condition) differs. Burnout is context-specific—usually tied to the professional environment—whereas depression is pervasive across all life domains.
| Feature | Occupational Burnout | Clinical Depression (MDD) |
|---|---|---|
| Primary Trigger | Chronic workplace stress/mismatch | Multifactorial (Genetic, Bio, Psych) |
| Emotional State | Cynicism and Depersonalization | Pervasive Sadness/Anhedonia |
| Response to Rest | Partial improvement with detachment | Minimal improvement with rest alone |
| Scope | Situational (Work-centric) | Global (Affects all life areas) |
Research into these distinctions is largely funded by public health grants and university-led initiatives, such as those found in PubMed archives. It is vital to note that while burnout is not a psychiatric disorder, it is a primary risk factor for developing one. The transition from burnout to depression often occurs when the individual loses a sense of agency, leading to “learned helplessness.”
Funding and Bias Transparency
Much of the current data on burnout is derived from longitudinal studies funded by national health institutes (such as the NIH in the US) and the World Health Organization. However, patients should be wary of “wellness” programs funded by corporations. These programs often emphasize “mindfulness” or “resilience training”—which shifts the burden of health onto the employee—rather than addressing the systemic workload issues that cause the HPA axis to fail. True clinical recovery requires a reduction in the allostatic load, not just a temporary masking of symptoms.
Contraindications & When to Consult a Doctor
While lifestyle adjustments and boundary-setting are primary interventions, certain “red flags” indicate that burnout has transitioned into a more severe medical crisis. You must seek immediate professional medical intervention if you experience:

- Suicidal Ideation: Any thoughts of self-harm or a feeling that the world would be better without you.
- Physical Collapse: Sudden, unexplained fainting, chest pain, or severe tachycardia (rapid heart rate) during non-stressful periods.
- Severe Cognitive Impairment: An inability to perform basic tasks, profound memory loss, or disorientation.
- Treatment Resistance: If sleep and time off do not alleviate the “flatness” after 2-4 weeks, you may be dealing with clinical depression or a thyroid dysfunction (hypothyroidism), which mimics burnout symptoms.
Avoid the use of unprescribed stimulants (e.g., excessive caffeine or “nootropics”) to combat burnout fatigue. These substances further stimulate the adrenal glands, potentially accelerating the crash into total HPA axis exhaustion.
The Path Toward Recovery
Recovery from burnout is not a linear process; it is a physiological recalibration. The goal is to lower the allostatic load and restore sensitivity to glucocorticoid receptors. This is achieved through a combination of “radical detachment” from the stressor, regulated sleep hygiene to reset the circadian rhythm, and low-intensity movement to clear systemic inflammation.
As we move further into 2026, the medical community is shifting toward a “Preventative Occupational Health” model. The focus is moving away from treating the exhausted individual and toward auditing the toxic environments that create them. Until then, recognizing the biological reality of your exhaustion is the first step toward clinical recovery.
References
- World Health Organization (WHO). ICD-11 Classification of Burnout as an Occupational Phenomenon.
- The Lancet. “Chronic Stress and the Cardiovascular System: A Longitudinal Analysis.”
- JAMA Psychiatry. “Differential Diagnosis: Occupational Burnout vs. Major Depressive Disorder.”
- PubMed Central. “HPA Axis Dysregulation and Glucocorticoid Receptor Resistance in Chronic Stress.”

