Spanish health authorities are currently managing the disembarkation of passengers from a cruise ship following a Hantavirus outbreak. While typically transmitted via rodent excreta, this event has triggered rigorous screening to prevent community spread. Coordinated efforts between the WHO and EU health agencies aim to isolate cases and monitor exposed travelers.
This situation is an epidemiological anomaly. Hantaviruses are traditionally zoonotic, meaning they jump from animals to humans, and rarely spread between people. The emergence of a cluster on a cruise ship—a closed environment—raises urgent questions about the source of infection: was there a systemic rodent infestation in the ship’s ventilation, or are we witnessing a rare instance of human-to-human transmission? For the global traveling public, this underscores the vulnerability of high-density transit hubs to rare pathogens.
In Plain English: The Clinical Takeaway
- Not a Common Cold: Hantavirus is a severe respiratory or renal disease, not a typical flu, and requires immediate hospital intervention.
- Rodent Risk: Most infections occur by breathing in dust contaminated with rodent urine or droppings; it is not typically “contagious” like COVID-19.
- Early Warning: High fever combined with sudden shortness of breath after travel to endemic areas is a medical emergency.
The Pathophysiology of Capillary Leak Syndrome
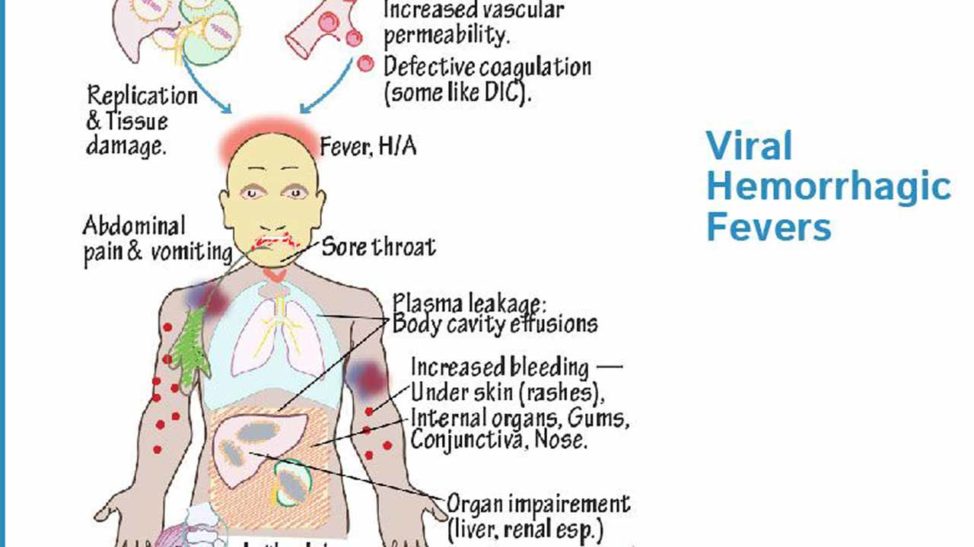
To understand why Hantavirus is so dangerous, we must examine its mechanism of action—the specific biochemical process the virus uses to cause disease. Hantaviruses target the vascular endothelium, which is the single layer of cells lining all blood vessels in the body.
The virus does not necessarily destroy these cells; instead, it disrupts the “tight junctions” that keep blood and fluids inside the vessels. This leads to capillary leak syndrome, a condition where plasma leaks out of the bloodstream and into the surrounding tissue. When this happens in the lungs, it results in Hantavirus Pulmonary Syndrome (HPS), effectively causing the patient to drown in their own fluids. When it occurs in the kidneys, it manifests as Hemorrhagic Fever with Renal Syndrome (HFRS).
This systemic failure is why supportive care is the only current treatment. Because there is no widely available antiviral drug specifically approved for Hantavirus, clinicians rely on extracorporeal membrane oxygenation (ECMO)—a machine that breathes and pumps blood for the patient—to keep them alive while the immune system fights the virus.
Zoonotic Jump vs. Human-to-Human Transmission
The primary concern for the Spanish Ministry of Health and the WHO is determining the transmission vector. In 99% of cases, Hantavirus is contracted via aerosolization—inhaling microscopic particles of dried rodent waste. However, the Andes virus strain, primarily found in South America, has demonstrated the ability for human-to-human transmission through close contact.
“The critical priority in any cruise-ship cluster is distinguishing between a common-source exposure—such as a contaminated galley or ventilation system—and a chain of human transmission. The latter would fundamentally change our quarantine protocols for disembarking passengers,” states Dr. Aris Katzourakis, an evolutionary biologist specializing in viral genomic surveillance.
The presence of a passenger on a KLM flight in Johannesburg further complicates the geo-epidemiological map. This suggests that the virus may have traveled across continents before the outbreak was recognized, necessitating a coordinated response between the European Medicines Agency (EMA) and South African health authorities to trace secondary contacts.
| Clinical Feature | Hantavirus Pulmonary Syndrome (HPS) | Hemorrhagic Fever with Renal Syndrome (HFRS) |
|---|---|---|
| Primary Target Organ | Lungs (Alveoli) | Kidneys (Renal Tubules) |
| Key Symptom | Rapid-onset respiratory failure | Acute kidney injury & hemorrhage |
| Common Geography | North and South America | Europe and Asia |
| Mortality Rate | High (Approx. 35% – 40%) | Variable (1% – 15%) |
Global Surveillance and the EMA Framework
The management of this outbreak falls under the International Health Regulations (IHR) overseen by the WHO. In Europe, the EMA and the European Centre for Disease Prevention and Control (ECDC) coordinate the “Early Warning and Response System” (EWRS). This allows Spain to share real-time genomic sequencing of the virus with other EU member states to ensure that hospitals in neighboring countries can recognize the symptoms quickly.
Funding for the ongoing surveillance of these strains is primarily provided by government public health grants and the Global Health Security Agenda. There is currently no private pharmaceutical “fast-track” for a Hantavirus vaccine because the virus does not typically cause the massive, sustained outbreaks seen with influenza or coronaviruses, making it a low priority for venture-capital-backed biotech firms.
For passengers currently in quarantine, the focus is on active surveillance—the process of proactively checking for symptoms rather than waiting for the patient to report them. This is vital because the prodromal phase (the early period of vague symptoms) can be easily mistaken for a common cold or mild COVID-19.
Contraindications & When to Consult a Doctor
While Hantavirus cannot be “prevented” with a pill, certain individuals are at higher risk for severe outcomes. Patients with pre-existing chronic obstructive pulmonary disease (COPD), congestive heart failure, or severe renal impairment are more likely to succumb to capillary leak syndrome due to their diminished physiological reserve.
Seek immediate emergency medical care if you experience:
- Sudden shortness of breath or difficulty breathing (dyspnea) following travel.
- High fever accompanied by severe muscle aches in the thighs, hips, and back.
- A drop in blood pressure or extreme dizziness.
- Decreased urine output, which may indicate renal distress.
Avoid using over-the-counter immunosuppressants or unverified “immune-boosting” supplements during the incubation period, as these can interfere with the body’s natural T-cell response required to clear the viral load.
The Future of Closed-Environment Biosafety
This incident serves as a stark reminder that our global connectivity often outpaces our diagnostic speed. The time lag between the initial infection on the cruise ship and the disembarkation in Spain highlights a gap in maritime health screening. Moving forward, People can expect the EMA and WHO to push for more stringent environmental audits of cruise vessels, focusing on rodent eradication and air filtration systems.

the resolution of this outbreak will depend on genomic tracing. If the virus is found to be a non-contagious strain, the panic will subside quickly. If, however, a mutation allowing for efficient human-to-human transmission is confirmed, we will need to rewrite the public health playbook for zoonotic spillover events in the 21st century.

