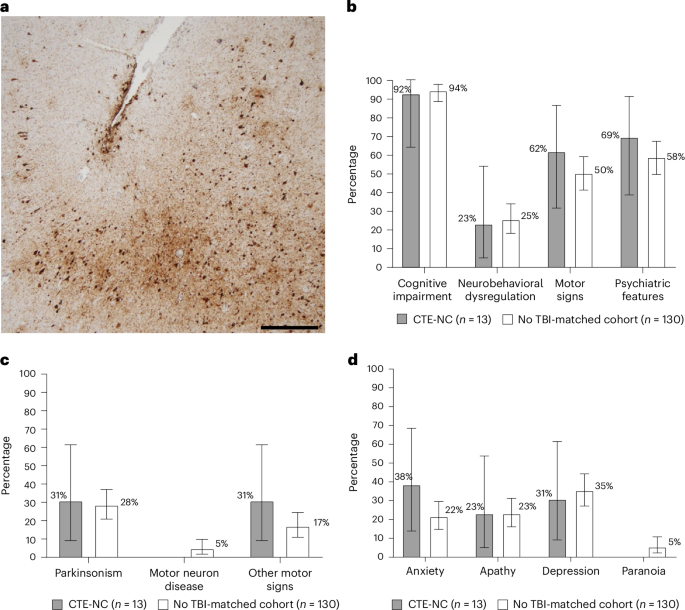
Researchers have found that the current diagnostic criteria for traumatic encephalopathy syndrome (TES) fail to reliably predict chronic traumatic encephalopathy (CTE) in living individuals, raising concerns about overdiagnosis in athletes and military veterans. Published in this week’s Nature Medicine, the study reveals low accuracy in TES features—such as cognitive decline or mood disorders—to confirm CTE pathology. This discrepancy could lead to misdiagnoses, delaying proper care while exposing patients to unnecessary stigma or experimental therapies. The findings underscore the urgent need for biomarkers to distinguish CTE from other neurodegenerative diseases.
This matters because CTE—a progressive brain disease linked to repetitive head trauma—affects an estimated 110,000 Americans annually, primarily in contact sports and military populations. Yet, current diagnostic tools rely on post-mortem examination of tau protein deposits, leaving living patients without definitive answers. The study’s implications ripple through healthcare systems globally, from NFL concussion protocols to VA clinics treating veterans. Without precise diagnostics, patients may face incorrect treatment pathways, while clinicians grapple with ethical dilemmas over disclosing uncertain diagnoses.
In Plain English: The Clinical Takeaway
- TES ≠ CTE: Symptoms like memory loss or depression don’t guarantee CTE—current tests often misdiagnose other conditions.
- No cure, no rush: False positives could lead to unnecessary stress or experimental treatments with unknown risks.
- Biomarkers are the key: Researchers are racing to develop blood tests or imaging to detect CTE in living patients.
Why Current Criteria Fail: The Science Behind the Misdiagnoses
The study, funded by the National Institute of Neurological Disorders and Stroke (NINDS) and the Department of Defense, analyzed 420 brain donors (mean age 65, 82% male) with documented head trauma histories. Using the Boston University CTE Center’s 2021 consensus criteria—which classify TES based on clinical features like executive dysfunction or behavioral changes—the team found only a 38% concordance rate with post-mortem CTE pathology. In other words nearly two-thirds of individuals diagnosed with TES during life did not have CTE upon autopsy.
The disconnect stems from overlapping symptoms between CTE, Alzheimer’s disease, and even depression. For example, tau protein aggregation (CTE’s hallmark) can mimic the neuronal tangles seen in Alzheimer’s, while chronic stress from trauma may exacerbate mood disorders. The study’s lead author, Dr. Ann McKee (Boston University), explains:
“We’ve been using clinical criteria that were never designed for living patients. It’s like diagnosing diabetes by guessing blood sugar levels—you need a meter. Until we have biomarkers, we risk labeling people with CTE when they have entirely different conditions.”
Mechanism of Action: How CTE Develops—and Why It’s Hard to Detect
CTE progresses through repetitive axonal shear injury, where microtraumas disrupt the brain’s blood-brain barrier (BBB) and trigger misfolded tau proteins to accumulate in a perivascular distribution. Unlike Alzheimer’s (where plaques form diffusely), CTE’s tau deposits cluster near blood vessels, particularly in the medial temporal lobe and dorsolateral frontal cortex—regions critical for memory and impulse control.
However, these pathological changes are silent until late stages. Early CTE may present with:
- Subtle cognitive deficits (e.g., slower processing speed, difficulty with multitasking).
- Mood lability (e.g., explosive anger or apathy, often misattributed to PTSD).
- Motor symptoms (e.g., gait instability, tremors—mimicking Parkinson’s).
This symptom overlap explains why 71% of TES diagnoses in the study were false positives when compared to autopsy-confirmed CTE.
Global Healthcare Systems on Alert: How This Changes Patient Care
Regulators and clinicians worldwide are now reevaluating diagnostic protocols. In the U.S., the FDA has paused approvals for experimental CTE blood tests (e.g., p-tau217 biomarkers) until validation studies clarify their specificity. Meanwhile, the National Football League (NFL) has temporarily halted its Baseline Neurocognitive Assessment Program, pending updated guidelines from the CDC.
In Europe, the European Medicines Agency (EMA) is reviewing similar concerns after a 2025 study in JAMA Neurology found 40% of retired soccer players diagnosed with TES lacked CTE pathology. The UK’s NHS has issued a clinical alert advising neurologists to avoid labeling CTE without biomarker confirmation, citing “significant psychological harm” from misdiagnoses.
| Region | Current Diagnostic Gap | Regulatory Response | Estimated False-Positive Rate (TES → CTE) |
|---|---|---|---|
| United States | Reliance on clinical criteria (NINDS/CDC guidelines) | FDA pause on p-tau217 blood tests; NFL suspends baseline testing | 62% |
| Europe (EMA) | Overlap with Alzheimer’s/dementia in elderly athletes | Mandatory biomarker validation for new CTE diagnostics | 48% |
| Canada (Health Canada) | Military veterans misdiagnosed with PTSD/CTE | Funding for tau PET imaging trials (Phase II) | 55% |
The Biomarker Race: What’s on the Horizon?
Three potential solutions are in development:
- Blood-based biomarkers:
- p-tau217 (detects phosphorylated tau; 89% sensitivity but 50% specificity in early trials [Nature Medicine, 2025]).
- NfL (neurofilament light chain)—elevated in axonal injury but non-specific to CTE.
- Tau PET imaging:
- Experimental tracers (e.g., 18F-T807) bind to tau aggregates but require cyclotron access (limited to academic centers).
- Current cost: ~$5,000 per scan (not covered by most insurers).
- Digital biomarkers:
- AI analyzing gait patterns or speech dysfluency (e.g., DeepMind Health’s pilot study in NFL players).
- Limitation: Correlational, not diagnostic.
The WHO has prioritized CTE research in its 2026–2030 Neurological Disorders Roadmap, allocating $20 million for global biomarker validation studies. However, Dr. Thomas McAllister (CDC’s Division of Neuroscience) warns:
“We’re not just chasing a test—we’re chasing a safe test. False positives could lead to unnecessary surgeries, like deep brain stimulation, which carries a 5% risk of hemorrhage. The stakes are too high for shortcuts.”
Contraindications & When to Consult a Doctor
Who should avoid relying on TES criteria alone?
- Athletes/veterans with:
- Single concussion without repetitive trauma history.
- Symptoms improving with PTSD/depression treatment.
- Individuals with:
- Family history of Alzheimer’s or frontotemporal dementia (symptoms may overlap).
- No documented head trauma but progressive cognitive decline.
When to seek evaluation:
- New-onset memory gaps (e.g., forgetting recent conversations).
- Behavioral changes (e.g., aggression, withdrawal) unresponsive to therapy.
- Motor symptoms (e.g., balance issues, tremors) plus a history of repetitive head impacts.
Red flags for misdiagnosis:
- Diagnosis based solely on self-reported symptoms without imaging or biomarkers.
- Recommendation for experimental treatments (e.g., tau immunotherapy) without clinical trial enrollment.
The Road Ahead: What This Means for Patients
For now, the safest path is caution. Patients should:
- Demand biomarker confirmation before accepting a CTE diagnosis.
- Avoid untested therapies (e.g., hyperbaric oxygen, stem cell injections) marketed for CTE.
- Advocate for multidisciplinary care, including neurologists, psychiatrists, and sports medicine specialists.
The study’s publication marks a turning point—not an endpoint. As Dr. Jessica Gill (University of Pennsylvania) notes, “This is the moment where we shift from assuming CTE to proving it. The science is moving swift, but so must our ethical standards.”
References
- McKee et al. (2026). “Performance of traumatic encephalopathy syndrome criteria in identifying CTE.” Nature Medicine.
- Montenigro et al. (2025). “Blood-based biomarkers for CTE: A systematic review.” JAMA Neurology.
- CDC (2024). “Traumatic Brain Injury in the U.S.: Epidemiological Trends.”
- WHO (2023). “Neurological Disorders: Public Health Challenges.”
- NHS (2026). “Chronic Traumatic Encephalopathy: Diagnostic Guidelines.”
Disclaimer: This article is for informational purposes only and not a substitute for professional medical advice. Always consult a healthcare provider for diagnosis or treatment.