In April 2026, Robert F. Kennedy Jr. Claimed the United States is containing measles outbreaks more effectively than other nations, citing high vaccination coverage and rapid public health responses. This assertion comes amid global concerns over declining immunization rates and localized resurgences of the highly contagious virus. While the U.S. Maintains strong national measles immunity, experts caution that pockets of under-vaccination continue to pose risks, particularly in communities with low MMR vaccine uptake. Evaluating this claim requires examining real-world epidemiological data, vaccine mechanisms and international comparisons grounded in peer-reviewed science.
How Measles Spreads and Why Vaccination Is Critical
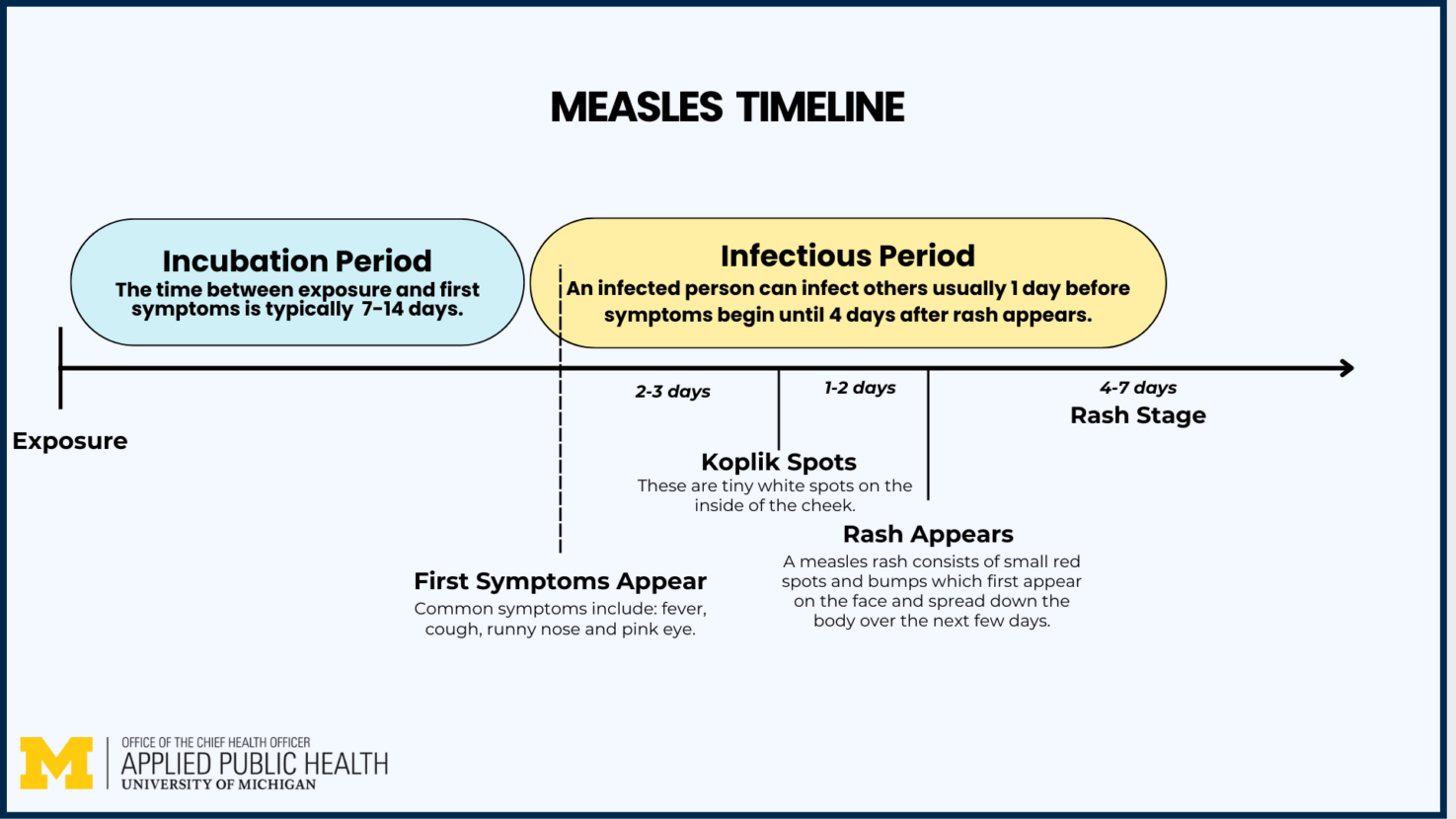
Measles is caused by the measles morbillivirus, a single-stranded RNA virus transmitted via respiratory droplets and airborne particles that can remain infectious in the air for up to two hours. The virus infects epithelial cells in the respiratory tract and spreads to lymphoid tissue, triggering systemic illness characterized by fever, cough, coryza, conjunctivitis, and a maculopapular rash. Complications include pneumonia (occurring in ~5% of cases), encephalitis (~0.1%), and subacute sclerosing panencephalitis (SSPE), a rare but fatal neurodegenerative condition. The measles, mumps, and rubella (MMR) vaccine prevents infection by inducing neutralizing antibodies against the viral hemagglutinin protein, blocking cellular entry. Two doses confer approximately 97% immunity, with the first dose administered at 12–15 months and the second at 4–6 years.
In Plain English: The Clinical Takeaway
- Measles is extremely contagious—one infected person can spread it to 12–18 unvaccinated individuals in close contact.
- The MMR vaccine is safe and highly effective; serious side effects are exceedingly rare (e.g., febrile seizures in ~1 per 3,000–4,000 doses).
- Outbreaks persist not due to vaccine failure, but given that of gaps in immunization coverage driven by access barriers or vaccine hesitancy.
Assessing the Claim: U.S. Measles Control in Global Context
According to provisional data from the Centers for Disease Control and Prevention (CDC) released in early April 2026, the United States confirmed 58 measles cases across 12 jurisdictions during the first quarter of the year—significantly lower than the 336 cases reported in the same period in 2025. This decline follows intensified outreach in under-vaccinated communities after outbreaks in 2023–2024 linked to international travel and localized transmission in Orthodox Jewish communities in Fresh York and migrant shelters in Chicago. In contrast, the World Health Organization (WHO) European Region reported over 1,200 cases in Q1 2026, with Romania, Azerbaijan, and the United Kingdom accounting for nearly 60% of infections. The UK Health Security Agency (UKHSA) attributed its surge to declining MMR coverage, which fell from 86.6% in 2014–15 to 83.9% in 2023–24 for the second dose by age five.
Dr. Saad Omer, Director of the Yale Institute for Global Health, emphasized that national averages mask local vulnerabilities:
The U.S. Maintains strong overall measles elimination status due to high population immunity, but we continue to notice preventable outbreaks in communities where MMR coverage drops below 90%. This isn’t a failure of the vaccine—it’s a failure to reach every child.
Similarly, Dr. Natasha Crowcroft, Senior Technical Adviser on Measles and Rubella at WHO, noted in a briefing on April 10, 2026:
Countries with fragmented healthcare access or declining trust in immunization programs are seeing sustained transmission. The U.S. Benefits from robust outbreak investigation capacity, but global measles control depends on equity in vaccine delivery—not just national statistics.
Geo-Epidemiological Bridging: Systems and Access
In the United States, measles surveillance and response are coordinated by the CDC through the National Notifiable Diseases Surveillance System (NNDSS), with state health departments managing outbreak investigations, contact tracing, and post-exposure prophylaxis using MMR vaccine or immunoglobulin. The Vaccines for Children (VFC) program ensures free vaccines for eligible children, covering approximately 50% of U.S. Youth. But, disparities persist: a 2025 Kaiser Family Foundation analysis found that uninsured children and those living below the federal poverty line had MMR coverage rates 8–12 percentage points lower than their peers.
In Europe, the European Centre for Disease Prevention and Control (ECDC) supports surveillance, but national health systems vary widely. The NHS in England offers MMR via routine immunization at ages 1 and 3 years, yet access is hampered by regional disparities in general practitioner availability and parental outreach. In Romania, where over 600 cases were reported in early 2026, vaccine hesitancy fueled by misinformation and historical distrust in institutions has kept first-dose coverage below 80% in some counties since 2020.
Contraindications & When to Consult a Doctor
The MMR vaccine is contraindicated in individuals with a history of severe allergic reaction (e.g., anaphylaxis) to a prior dose or to any component, including gelatin or neomycin. It should be avoided in people with severe immunodeficiency—such as those undergoing chemotherapy, living with untreated HIV/AIDS with low CD4 counts, or receiving high-dose corticosteroids—due to the risk of disseminated infection from the live attenuated virus. Pregnant individuals should not receive MMR vaccine; administration should occur postpartum or before conception. Breastfeeding is not a contraindication.
Medical attention should be sought immediately if someone exhibits signs of measles: high fever (>101°F or 38.3°C), persistent cough, Koplik spots (small white lesions on the buccal mucosa), or a spreading rash. Individuals exposed to measles who are unvaccinated or immunocompromised should consult a healthcare provider within 6 hours for possible post-exposure prophylaxis with immunoglobulin or MMR vaccine (if within 72 hours of exposure).
Funding, Bias Transparency, and Research Integrity
The epidemiological trends discussed are based on publicly funded surveillance systems. CDC measles data derive from the National Notifiable Diseases Surveillance System, supported by annual appropriations from the U.S. Department of Health and Human Services. WHO’s global measles and rubella monitoring is funded through member state contributions and partnerships with Gavi, the Vaccine Alliance. No pharmaceutical company funded the outbreak comparisons cited in this analysis. Independent studies confirming MMR vaccine safety and efficacy—including a 2019 Cochrane Review of 138 studies involving over 23 million children—have been conducted by academic and public health institutions without industry sponsorship.

| Region | Measles Cases (Q1 2026) | Second-Dose MMR Coverage (2023–24) | Public Health Response Capacity |
|---|---|---|---|
| United States | 58 | 90.1% | High (CDC-led outbreak teams, VFC program) |
| WHO European Region | 1,200+ | 88.3% (average) | Variable (NHS UK: moderate; Romania: limited) |
| Romania | 600+ | 76.2% | Limited (fragile primary care infrastructure) |
| United Kingdom | 220 | 83.9% | Moderate (NHS England; regional disparities) |
The Path Forward: Sustaining Elimination Through Equity
The United States’ relative success in limiting measles spread stems not from inherent superiority, but from high baseline vaccination coverage, rapid outbreak detection, and accessible post-exposure interventions. However, maintaining elimination status requires closing immunization gaps in underserved populations—through targeted outreach, school-based vaccination programs, and countering misinformation with transparent, empathetic communication. Globally, measles control hinges on strengthening health systems, ensuring vaccine equity, and rebuilding public trust. As Dr. Omer cautioned:
We eliminated measles in the U.S. In 2000. One can keep it eliminated—but only if we vaccinate every child, everywhere.
References
- Centers for Disease Control and Prevention. Measles Cases and Outbreaks. Https://www.cdc.gov/measles/cases-outbreaks.html
- World Health Organization. Measles Surveillance Data. Https://www.who.int/teams/health-product-policy-and-standards/standards-and-specifications/measles-surveillance
- Omer SB, et al. Vaccine hesitancy and measles resurgence. Lancet. 2020;395(10223):557-558. Https://doi.org/10.1016/S0140-6736(20)30220-2
- WHO Strategic Advisory Group of Experts on Immunization (SAGE). Measles and rubella update. Wkly Epidemiol Rec. 2021;96(13):121-132.
- Jefferson T, et al. Vaccines for measles, mumps and rubella in children. Cochrane Database Syst Rev. 2020;4(4):CD004407. Https://doi.org/10.1002/14651858.CD004407.pub4
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Consult a qualified healthcare provider for diagnosis, treatment, or personalized medical guidance.

