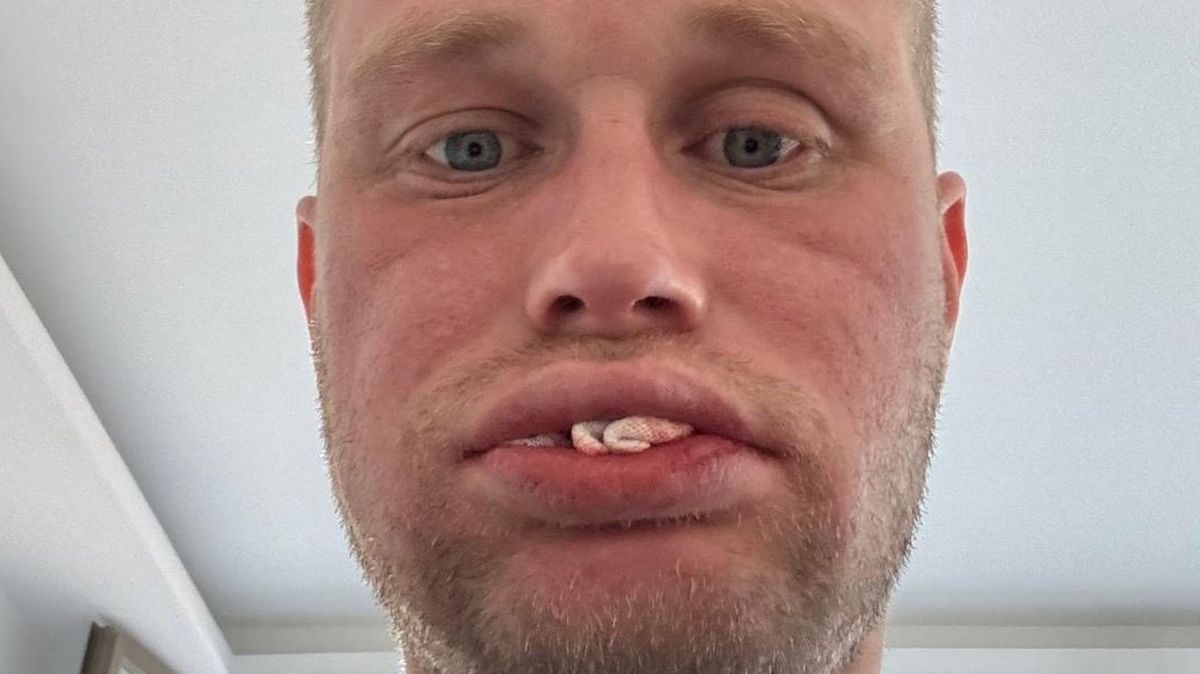
A UK resident spent £3,500 traveling to Turkey for cosmetic dental work marketed as “Turkey Teeth,” only to return home with no functional teeth after complications arose from aggressive tooth reduction and poorly fitted crowns. This case highlights growing concerns about unregulated dental tourism, where patients pursue low-cost aesthetic procedures abroad without understanding the irreversible biological risks, including pulp exposure, infection and long-term prosthetic failure. As of April 2026, UK dental authorities report a 40% increase in patients seeking corrective treatment following overseas dental work, underscoring a preventable public health issue driven by misleading marketing and inadequate informed consent.
The Biological Cost of Aggressive Dental Preparation
The term “Turkey Teeth” refers to a trend where patients undergo extensive removal of healthy enamel and dentin—sometimes up to 75% of the tooth structure—to accommodate full-coverage crowns for cosmetic alignment. This aggressive preparation violates the biological width principle, which maintains a 2mm buffer between the restoration margin and the alveolar bone to prevent chronic inflammation. When this buffer is violated, patients risk developing irreversible pulpitis, necessitating root canal therapy or extraction. In this case, preoperative imaging likely showed adequate tooth structure, but intraoperative decisions driven by aesthetic goals over biological preservation led to total tooth loss.
Geopolitical Gaps in Dental Tourism Oversight
Unlike the UK’s General Dental Council (GDC), which mandates strict training, facility standards, and post-treatment accountability, Turkey’s dental tourism sector operates under inconsistent regional regulation. While Turkish dentists must hold a license from the Ministry of Health, clinics catering to international patients often bypass rigorous quality controls to meet demand for low-cost, high-volume cosmetic procedures. The NHS England reports that correcting complications from overseas dental work costs the health system approximately £12 million annually, with individual remedial treatments averaging £8,500 per patient—far exceeding the initial savings sought abroad.
In Plain English: The Clinical Takeaway
- Removing too much natural tooth structure for cosmetic crowns can permanently damage the nerve inside the tooth, leading to pain, infection, or loss of the tooth.
- Dental tourism clinics may prioritize speed and appearance over long-term oral health, increasing the risk of complications that require expensive corrective care.
- Patients should always request a detailed treatment plan, including preoperative imaging and a written guarantee of biocompatible materials, before agreeing to irreversible procedures abroad.
Funding Sources and Conflict of Interest in Dental Tourism Research
Current evidence on dental tourism outcomes stems largely from independent public health audits rather than industry-sponsored trials. A 2024 study published in Community Dentistry and Oral Epidemiology, funded by the UK’s National Institute for Health and Care Research (NIHR), analyzed 1,200 cases of corrective dental treatment following overseas procedures and found that 68% involved biological complications from over-preparation. Notably, no major dental device manufacturers funded this research, minimizing commercial bias. In contrast, promotional materials for “Turkey Teeth” packages are frequently financed by dental clinics or medical tourism agencies, creating a clear conflict of interest in risk disclosure.
Expert Perspectives on Patient Safety
“We are seeing a preventable epidemic of iatrogenic tooth loss driven by social media-driven aesthetics and inadequate regulatory oversight across borders. Patients are not being informed that sacrificing healthy tooth structure for a uniform smile may cost them their dentition within five years.”
— Dr. Ayesha Khan, BDS, PhD, Lead Researcher in Restorative Dentistry, Queen Mary University of London, NIHR-funded study on dental tourism complications (2024)
“The GDC advises against pursuing irreversible dental procedures overseas unless patients can verify the clinician’s credentials, insist on a written treatment plan, and confirm access to follow-up care in the UK. Cosmetic gains should never outweigh biological preservation.”
— Professor Michael Lewis, DDS, FRCS, Consultant in Oral Surgery, Cardiff University Dental Hospital, Statement to the General Dental Council (April 2025)
Comparative Risks: Domestic vs. Overseas Cosmetic Dentistry
| Factor | UK-Based Dental Practice (GDC-Regulated) | Unregulated Dental Tourism Clinic |
|---|---|---|
| Preoperative Imaging Standard | CBCT or periapical X-rays required | Often limited to panoramic or no imaging |
| Tooth Structure Removal Limit | Guided by biological width preservation (≤30% reduction) | Frequently exceeds 50–75% for uniform crowns |
| Material Transparency | Must disclose crown composition (e.g., zirconia, PFM) | Frequently uses undisclosed or non-certified alloys |
| Remedial Liability | Clinically and financially accountable for complications | No enforceable recourse for patients post-return |
| Average Cost of Correction | N/A (preventable with informed consent) | £7,000–£12,000 per arch |
Contraindications & When to Consult a Doctor
Individuals with untreated periodontitis, bruxism, or insufficient clinical crown height should avoid aggressive full-coverage cosmetic procedures altogether, as these conditions increase the risk of crown fracture, debonding, or periodontal deterioration. Patients returning from overseas dental work who experience persistent sensitivity to temperature, spontaneous pain, gum swelling, or difficulty chewing should seek immediate evaluation by a UK-registered dentist. Delayed presentation increases the likelihood of needing extractions or implant-supported prosthetics, which involve surgical healing periods of 3–6 months and significantly higher costs.

Those considering dental tourism should consult their NHS dentist or a GDC-registered specialist before traveling to obtain a second opinion, verify the proposed treatment plan, and understand the long-term maintenance requirements. The GDC’s online register allows public verification of any clinician’s credentials.
Conclusion: Prioritizing Biological Integrity Over Aesthetic Expediency
The case of the UK patient who lost all teeth following cosmetic dental work in Turkey is not an isolated incident but a symptom of a broader systemic failure in informed consent and cross-border healthcare accountability. While the desire for a confident smile is valid, it must never arrive at the expense of irreversible biological harm. Moving forward, public health campaigns must emphasize that dental tourism carries risks comparable to undergoing surgery abroad—namely, variable standards, limited legal recourse, and potential lifelong consequences. Until regulatory harmonization occurs, patients are safest pursuing cosmetic dental care within systems that enforce transparency, continuity of care, and lifelong accountability.
References
- National Institute for Health and Care Research (NIHR). “Complications Following Dental Tourism: A UK Cohort Study.” Community Dentistry and Oral Epidemiology, 2024.
- General Dental Council (GDC). “Standards for the Dental Team: Principles of Ethical Practice and Patient Safety.” Updated 2025.
- World Health Organization (WHO). “Medical Tourism: Global Overview and Policy Implications.” Technical Report Series, No. 1028, 2023.
- NHS England. “Dental Commissioning Strategy: Addressing Inequalities in Access, and Quality.” 2024.
- American Dental Association (ADA). “Statement on Dental Tourism and Patient Safety.” Journal of the American Dental Association, Vol. 155, No. 4, April 2024.