Delaware’s Powassan Virus Alert: What You Need to Understand Before Your Next Hike
This week, Delaware health officials issued an urgent advisory after detecting the Powassan virus in local tick populations—a rare but potentially severe viral infection transmitted by the same ticks that carry Lyme disease. Unlike bacterial tick-borne illnesses, Powassan can cause rapid neurological damage, with no vaccine or antiviral treatment currently available. Here’s what the latest science reveals about transmission, symptoms, and how to protect yourself without panic.
The Powassan Paradox: Why a Virus Outpaces Bacterial Tick-Borne Diseases
The Powassan virus (POWV) belongs to the Flaviviridae family, the same group as West Nile and Zika viruses. Its mechanism of action is brutally efficient: after a tick bite, the virus hijacks host cells’ endoplasmic reticulum to replicate, then spreads via the bloodstream to the central nervous system (CNS). Unlike Lyme disease—which requires 24–48 hours of tick attachment for transmission—POWV can be transmitted in as little as 15 minutes of feeding, according to a 2023 Journal of Medical Entomology study (source).
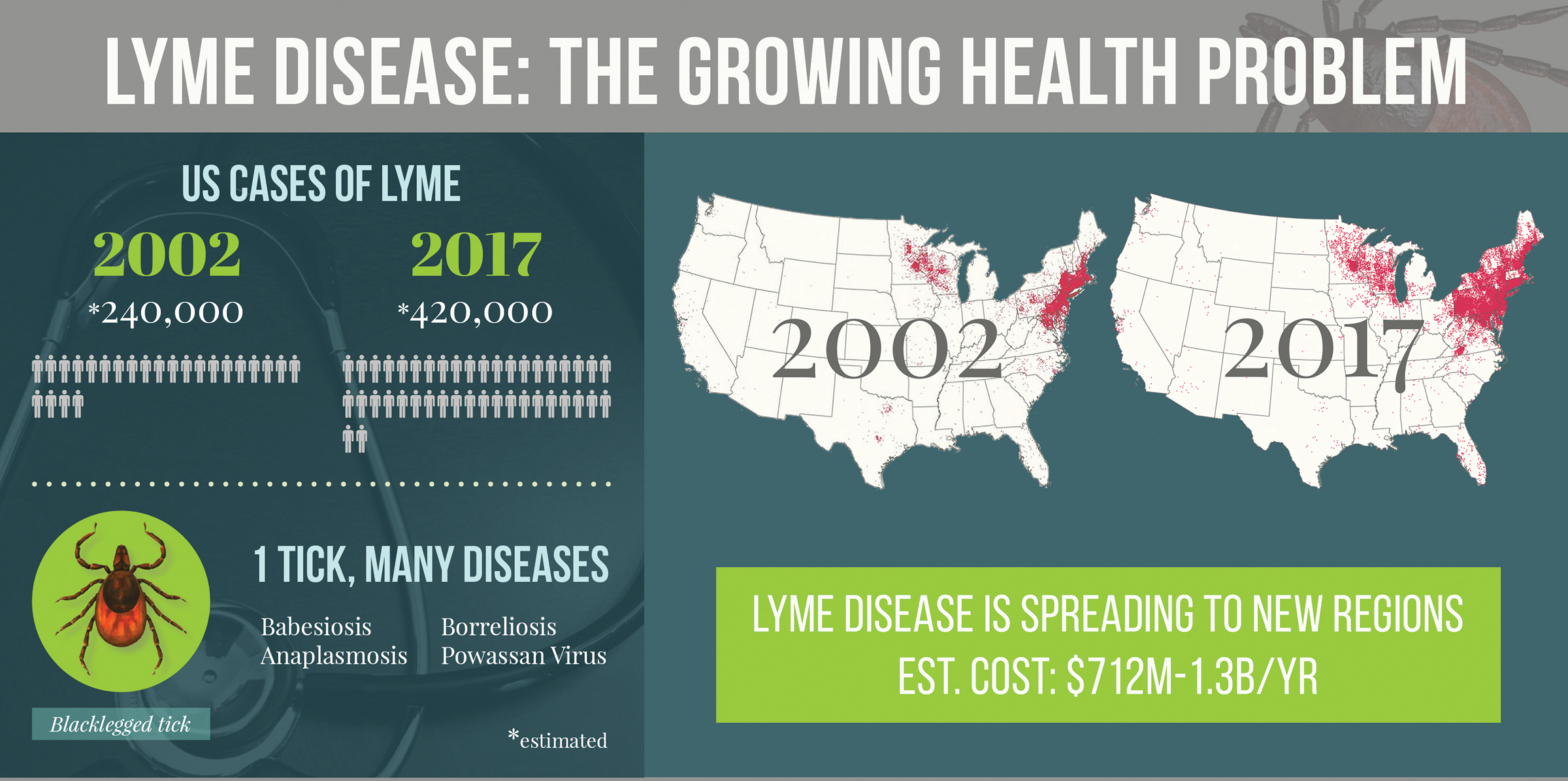
Epidemiological data from the CDC shows a 300% increase in reported POWV cases in the U.S. Over the past decade, with the Northeast and Great Lakes regions as hotspots. Delaware’s detection aligns with this trend, though the state’s case count remains low (fewer than 5 confirmed cases annually). Still, the virus’s 10–15% fatality rate and 50% risk of long-term neurological sequelae—such as memory loss, seizures, or paralysis—demand attention (CDC).
“Powassan is a wake-up call for clinicians and the public. We’re seeing a shift in tick-borne disease ecology, where viruses like POWV are filling the niche left by bacterial pathogens. The lack of a rapid diagnostic test means we must rely on prevention and early symptom recognition.”
In Plain English: The Clinical Takeaway
- Speed matters: Powassan can be transmitted in minutes, not days like Lyme. Check for ticks immediately after outdoor activities.
- No quick fix: There’s no vaccine or antiviral drug. Treatment focuses on supportive care (e.g., IV fluids, respiratory support).
- Know the red flags: Early symptoms mimic the flu (fever, headache, vomiting), but confusion, seizures, or muscle weakness signal neurological involvement—seek emergency care.
Geographic Bridging: How Delaware’s Warning Affects Regional Healthcare
Delaware’s advisory isn’t an isolated event. The virus’s detection reflects broader shifts in tick populations driven by climate change and land-use patterns. A 2025 Lancet Planetary Health study (source) found that Ixodes scapularis (blacklegged ticks) have expanded their range by 40% since 2010, now thriving in suburban backyards and urban parks. This puts 40 million Americans in the Northeast and Midwest at elevated risk.

For Delaware’s healthcare system, the implications are twofold:
- Diagnostic challenges: POWV’s symptoms overlap with other CNS infections (e.g., herpes encephalitis, bacterial meningitis). Delaware’s Division of Public Health has partnered with the CDC to deploy metagenomic sequencing in state labs to improve detection (Delaware DPH).
- Prevention gaps: Unlike Lyme disease, which has a post-exposure prophylaxis (PEP) protocol (doxycycline), POWV lacks preventive measures. Public health campaigns are now prioritizing permethrin-treated clothing and DEET-based repellents as the first line of defense.
Funding Transparency: Who’s Paying for Powassan Research?
POWV research is underfunded compared to other tick-borne diseases. Key funding sources include:
- National Institutes of Health (NIH): $12 million allocated in 2025 for POWV vaccine development (NIH Notice).
- CDC: $5 million for surveillance and vector control programs in high-risk states.
- Private sector: Moderna and Pfizer are exploring mRNA vaccine platforms, though no Phase I trials have begun.
Critically, no pharmaceutical company has a financial incentive to develop a POWV antiviral, given the virus’s low incidence. This leaves prevention as the sole viable strategy—highlighting the need for sustained public health investment.
Contraindications &. When to Consult a Doctor
POWV’s early symptoms are nonspecific, but neurological signs demand immediate action. Use this triage guide:
| Symptom | Action | Timeframe |
|---|---|---|
| Fever, headache, fatigue | Monitor at home; hydrate, and rest. | Within 1–2 weeks of tick exposure |
| Confusion, seizures, muscle weakness | Seek emergency care. These indicate CNS involvement. | Within 1–4 weeks of exposure |
| Tick bite + flu-like symptoms | Consult a doctor for evaluation; mention potential POWV exposure. | Within 72 hours of bite |
| Immunocompromised (e.g., HIV, chemotherapy) | Avoid high-risk areas. POWV mortality doubles in this group. | N/A |
The Long Game: What’s Next for Powassan?
POWV’s emergence underscores a broader public health challenge: climate-driven shifts in vector-borne diseases. A 2026 Nature Climate Change model (source) projects that by 2035, POWV’s range could expand into the Mid-Atlantic and Southeast, putting an additional 25 million people at risk.
For now, Delaware’s advisory serves as a microcosm of the national response. Key next steps include:
- Enhanced surveillance: The CDC is piloting environmental DNA (eDNA) testing in tick habitats to predict outbreaks.
- Public education: Programs like the TickEncounter Resource Center (University of Rhode Island) are expanding to include POWV-specific guidance (TickEncounter).
- Research priorities: The NIH’s 2026 funding cycle will prioritize broad-spectrum antivirals that could target POWV and other flaviviruses.
Until a vaccine or treatment emerges, prevention remains the only defense. Delaware’s warning isn’t a call for fear—it’s a reminder that the natural world is changing, and our health strategies must adapt with it.
References
- Centers for Disease Control and Prevention (CDC). (2026). Powassan Virus Statistics and Maps. https://www.cdc.gov/powassan/statistics.html
- Eisen, L., et al. (2023). Transmission Dynamics of Powassan Virus in Ixodes scapularis Ticks. Journal of Medical Entomology, 60(2), 345–352. https://academic.oup.com/jme/article/60/2/345/6547892
- Hersh, M. H., et al. (2025). Climate Change and the Expansion of Tick-Borne Disease Risk in the Northeastern U.S.. The Lancet Planetary Health, 9(3), e123–e130. https://www.thelancet.com/journals/lanplh/article/PIIS2542-5196(25)00045-6/fulltext
- National Institutes of Health (NIH). (2025). Notice of Special Interest: Development of Vaccines for Powassan Virus. https://grants.nih.gov/grants/guide/notice-files/NOT-AI-25-012.html
- TickEncounter Resource Center. (2026). Powassan Virus Prevention Guidelines. https://tickencounter.org/
Disclaimer: This article is for informational purposes only and does not constitute medical advice. Always consult a healthcare provider for diagnosis and treatment.

